EHR Costs Breakdown: Pricing, Hidden Fees, and Budgeting Tips
Today, it is almost impossible to imagine a healthcare facility without an EHR. From patient check-ins to post-recovery tracking, EHRs have permeated every nook and cranny, becoming an indispensable part of the healthcare ecosystem. However, like all technologies, EHRs come with their own costs, both direct and indirect, that healthcare organizations must consider.
Direct Costs
Contributing directly to the implementation, maintenance, and operation of EHRs, direct cots are more straightforward and are easier to predict. These include:
1. Software
EHR software can be either cloud-based or on-premise. Cloud-based systems typically require a subscription fee, while on-premise solutions involve a one-time licensing fee, incurring support and maintenance overheads.
2. Hardware Costs
EHR implementation requires hardware like servers, computers, tablets, and other specialized medical equipment that integrates with the system.
3. Data Migration
Data migration costs include converting paper records into digital formats and ensuring flawless interoperability between old and new systems. It also involves thorough testing to ensure integration aligns with healthcare providers’ existing workflows.
4. Training
A considerable amount of investment can go into training staff members on the new system, with periodic training updates as the system evolves, driving up expenses.
5. Customization
Customization is often needed to ensure EHR meets the clinic’s unique needs. From adjusting templates to hiring consultants for assistance, cost plays a key factor in the process.
Indirect Costs
Being equally important, indirect costs are unquantifiable, hidden, and accumulate over time. The most recurring of these include:
1. Productivity Loss
Adjusting to a new system takes time, often leading to a temporary dip in productivity for both clinicians and administrative staff.
2. Maintenance and Updates
While maintenance costs can sometimes be direct, indirect expenditures stem from system downtime, execution, and testing of software updates.
3. Compliance and Regulatory Requirements
Due to the sensitive nature of patient data, healthcare organizations must comply with strict regulatory standards (such as HIPAA in the U.S.), which can result in increased IT resource demands and higher audit costs.
4. Support Services
Beyond initial training, staff may require technical assistance over time. While some systems may include basic support, comprehensive or 24/7 support often incurs additional expenses.
5. Impact on Patient Care
Although EHRs are intended to enhance patient care, poor design or inadequate utilization by clinics can negatively impact patient outcomes.
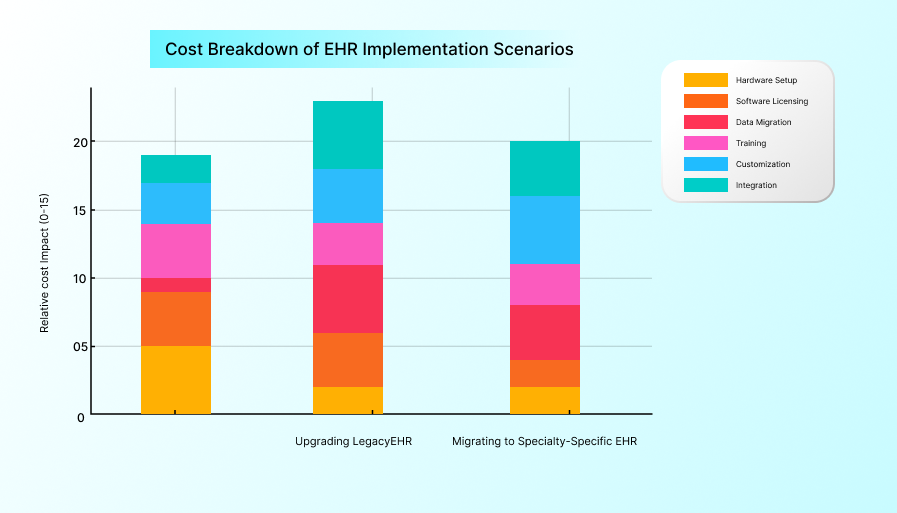
Even so, not all EHR implementations have similar costs. They vary significantly based on the practice size, patient volume, and implementation intent. Whether you’re a new clinic selecting your first EHR, upgrading a legacy system, or transitioning from a general EHR to a specialty-specific solution, each scenario involves different processes and pricing structures.
Below, we provide in-depth insights into how EHR implementation costs and onboarding processes vary for new clinics, practices with legacy systems, and facilities considering a switch. Also, to help you plan effectively, we conclude this article with our expert-recommended budgeting tips.
Launching a New Clinic
1. Initial Setup:
- Hardware: The investment for hardware infrastructure typically ranges from $10,000 to $50,000, depending on the clinic’s size and specific requirements.
- Software licensing or subscription fee: The software cost depends on the vendor and organization’s size. For example, Epic’s EHR system may cost around $1 million for smaller hospitals, with larger health systems facing fees of $10 million or more. In comparison, eClinicalWorks offers cloud-based EHR solutions starting at $449 per month per provider for the EHR-only package, while their EHR with Practice Management package is priced at $599 per month per provider.
Interested in knowing how OmniMD pricing beat the competition?
Give us a call now!
2. Customization
Customization costs for a new clinic can range from $2,000 to $10,000, depending on the complexity and extent of the modifications.
3. Training
Relying on the program’s length and depth, the cost can typically range from $1,000 to $5,000 per staff member.
4. Compliance and Security
Applying security protocols can cost between $5,000 to $20,000 annually. This includes expenses for encryption, regular security audits, and compliance checks. Additionally, for clinics adopting cloud-based EHR solutions, following a cloud security checklist ensures that patient data remains protected and meets regulatory standards.
Total Investment
On average, small practices might spend between $20,000 to $65,000, while mid-sized clinics could see costs ranging from $65,000 to $200,000.
Upgrading from a Legacy EHR System:
According to the Grand View Research, the web/cloud-based EHR segment dominated the North American market, holding an 83.28% share.Upgrading from an outdated EHR system comes with various costs, including data migration, integration, training, and potential productivity disruptions. Here’s an overview of what these expenses might entail:
1. Data Migration
Legacy systems store both structured data (such as patient demographics, appointments, and diagnoses) and unstructured data (like scanned documents and images). Extracting, cleaning, and migrating this data to match the new system’s structure can incur costs ranging from $50,000 to $250,000.
2. Integration
The cost of ensuring interoperability depends on the number of systems to integrate and the compatibility of those systems. If custom solutions are needed, the price can range anywhere from $20,000 to $150,000.
3. Staff Training
Training staff on using the new system, which can involve multiple sessions for different user groups such as physicians, nurses, and administrative staff, can cost between $10,000 and $50,000. This is based on how many staff members need training, how long the training will last, and whether the EHR vendor or an external consultant provides the training.
4. Downtime and Productivity Loss
During the transition, the system may experience periods of inaccessibility, and new users may encounter errors as they become familiar with it, potentially resulting in productivity losses ranging from $20,000 to $100,000.
Total Estimated Cost
Depending on the complexity of integration, migration, and the training required, the total cost for upgrading from a legacy system can range from $2,000,000 to $4,000,000.
Migrating from a Generic EHR to a Specialty-Specific Solution
Switching from a generic EHR to a specialty-specific solution incurs additional customization and integration costs. Here’s what you can expect:
1. Customization and Templates
Specialty EHRs are designed with structured reporting, patient documentation templates, and customizable examination forms, priced between $10,000 and $50,000.
2. Data Conversion
The cost of accurately mapping data from a generic EHR to a new specialty system can range from $15,000 to $40,000. This process includes reformatting and organizing existing patient records, as well as performing extensive testing and validation to ensure data integrity.
3. New Integrations
Specialty EHRs often require integrations with additional tools or systems that aren’t necessary with generic EHRs. The estimated cost for these integrations typically ranges from $10,000 to $40,000.
4. Training & Workflow Adjustment
Training costs include the creation of specialty-specific training materials and the time spent in training sessions. This ranges anywhere between $10,000 and $30,000.
Total Expenses
A general practice transitioning from a generic EHR to a specialty-specific solution could expect to spend anywhere from $50,000 to $100,000, depending on the specific needs for customization, integration, data conversion, and training.
In Essence
Costs vary widely, from launching a new clinic to upgrading from a legacy system and migrating to a specialty-specific solution. Thus, it’s essential to plan ahead for expenses.
Here’s How You Can Control EHR Expenses: A Conclusion
- Start small and scale up: Implement EHR in phases. Begin with basic features like patient records and billing, then gradually add advanced functionalities like scheduling or analytics as your budget allows.
- Choose cloud-based solutions: They typically have lower upfront costs and predictable subscription payments.
- Leverage government incentives: Check your eligibility and apply for government incentives such as the Medicare and Medicaid EHR Incentive Programs to offset some of the costs.
- Compare vendors and negotiate: Request proposals from multiple EHR vendors and compare their pricing. Don’t be afraid to negotiate on pricing, features, and payment terms to fit your budget.
- Proactively manage hidden costs: Prevent unexpected financial strain by keeping aside funds for training, data migration, or integration with other systems.
- Save on staff training: Instead of in-person training, consider online or vendor-provided training, which is often more affordable and flexible.
Frequently Asked Questions
The choice depends on your practice’s size, IT resources, and budget. If you are a small practice, cloud-based systems could be more affordable and easily scalable. On the other hand, on-premise systems can be a better option for larger practices looking for more control over data storage and security.
To estimate long-term costs, consider both direct and indirect expenses. It’s also important to factor in potential costs for future system expansions, integrations, and compliance with new regulations.
While transitioning to a new system often leads to downtime, careful planning and utilizing experienced vendors who offer migration support can minimize disruptions. smooth migration, read our latest blog here.
In such cases, audit the system for unexpected fees. Discuss any unclear charges with the vendor and negotiate a more predictable pricing model.

Uncover the True Cost of EHR!
Avoid hidden fees & budget smarter – get the full pricing breakdown now!

 Written by Neha Singh
Written by Neha Singh
 Reviewed by Shivani Joshi
Reviewed by Shivani Joshi