Get Paid in 29 Days with a Medical Billing Specialist Who Lives and Breathes Your Payers
One Revenue Cycle Specialist, dedicated exclusively to your practice. They work inside your EMR, know your payer mix inside out, and are backed by a full billing team you never had to hire. No overhead, no turnover, no ramp-up.
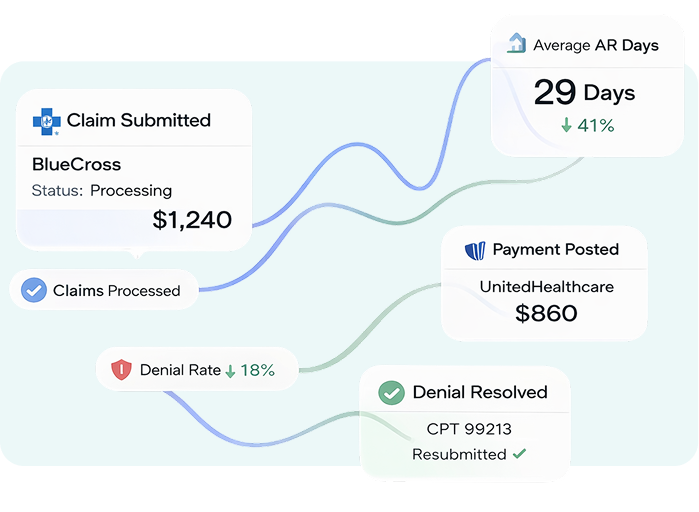
First-Pass Claim Acceptance
Net Denial Rate
Avg. Revenue Uplift in Year
Years Serving US Practices
Your Practice Is Running at Full Capacity, So Why Is Money Still Walking Out the Door?
Denials That Never Get Appealed
Two-thirds of denied claims are recoverable, but only when someone actively pursues them within the payer’s appeal window.

Eligibility Checked Too Late
A coverage issue caught before the appointment is a conversation. Caught after the claim is denied, it is a write-off.

AR Aging Past the Point of Recovery
After ninety days, average claim recovery rates drop below forty percent. After a hundred and twenty, most practices stop trying.

The Turnover Tax Nobody Talks About
Every time your biller leaves, three to six months of payer knowledge, workflow familiarity, and denial history walks out with them, and your collections feel it before the new hire is even up to speed.
We Work Across 20+ Specialties. And We Know the Difference Between All of Them.
Cardiology doesn’t bill like pediatrics. OB/GYN doesn’t code like urgent care. Your specialist is matched to your specialty, your payers, and your EMR from day one.
How OmniMD Works
Your Revenue Cycle Specialist isn’t shared, rotated, or managed through a queue. They show up for your practice every day, the same way a direct hire would. We just handle everything behind the scenes.
Revenue Cycle Specialist
With a minimum of five years working exclusively on US-based accounts, your specialist owns the entire billing cycle: payer relationships, AR performance, denial trends, and collections accountability. This is the person you call, the person who knows your practice inside out, and the person whose performance is measured against your revenue outcomes.
Certified Medical Coding Specialist
Credentialed through AAPC or AHIMA with specialty-specific experience across ICD-10, CPT, and HCPCS, your coding specialist ensures every claim is coded accurately and compliantly before it reaches the clearinghouse. Clean coding at the front end is the single most effective way to reduce denials downstream.
Eligibility Verification Coordinator
Running real-time eligibility verification before every scheduled encounter, your coordinator confirms active coverage, co-pay obligations, and prior authorization requirements through the clearinghouse, catching the issues that generate the most preventable denials in any practice.
Claims Submission Specialist
Every claim is scrubbed, batched, submitted, and tracked through the full clearinghouse pipeline. Rejections are flagged in real time and resubmitted the same day, so nothing sits waiting for someone to notice it.
Clearinghouse and EDI Specialist
Every transaction moving between your practice and your payers runs through a clearinghouse, and how that connection is managed determines how fast you get paid. Your specialist handles the full EDI transaction set: 837P claim files out, 835 remittance files back, 270/271 eligibility requests, and 276/277 claim status checks across Availity, Change Healthcare, Waystar, and all major clearinghouses. Transmission errors and batch failures are caught before they age into recovery problems.
Denial Management Analyst
Your denial management analyst goes further than correction and resubmission, identifying the payer-specific patterns behind recurring denials, building appeal strategies tailored to each payer’s documentation requirements, and implementing front-end workflow changes that prevent the same denial from landing on your account twice.
AR Recovery and Follow-Up Specialist
Every aging claim is pursued with structured, prioritized follow-up organized by balance, payer, and recovery probability. Nothing crosses sixty days without a documented action already taken on it.
Reporting and Analytics Manager
You receive the performance data that actually matters: denial rates by payer, AR aging breakdowns, collection ratios by provider, and monthly payer scorecards, delivered in the format and at the frequency you specify.
Let’s Get Started: From Signed Agreement to First Claims Out the Door in Seven Days
1
Specialist Matching
We match you with a Revenue Cycle Specialist based on your specialty, EMR platform, and payer mix, a deliberate match, not whoever happens to be available.
2
EMR and Clearinghouse Integration
Your specialist connects directly to your existing systems, already certified on your platform, with clearinghouse configurations and EDI connections confirmed before any claims move.
3
Eligibility and Payer Audit
We review your active payer contracts, enrollment status, and authorization workflows, and surface the gaps that have been quietly generating denials before we ever submit a claim.
4
First Claims Submitted
Within seven days of signing, clean claims are moving through the clearinghouse, and your specialist sends you a full kickoff report covering what has been set up, what has been found in your existing AR, and what the first thirty-day recovery plan looks like.
What a Year With OmniMD Medical Billing Experts Looks Like
29 Days
Average time-to-payment, compared to an industry average of forty-five to sixty days.
98.6%
First-pass claim acceptance rate through the clearinghouse on initial submission.
35%
Average revenue increase in Year 1 for practices transitioning from in-house billing.
97%
Denial appeal success rate on appeals filed and documented within thirty days of the original denial.
$1.8M
Average underpaid and denied claim recovery per practice in the first twelve months of engagement.
<2%
Net denial rate maintained consistently across all active OmniMD client accounts.





