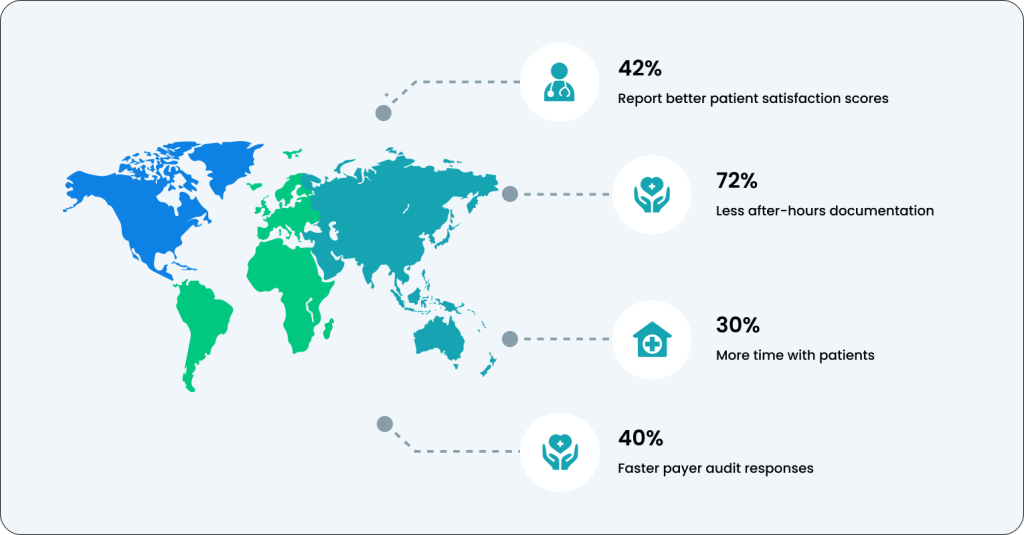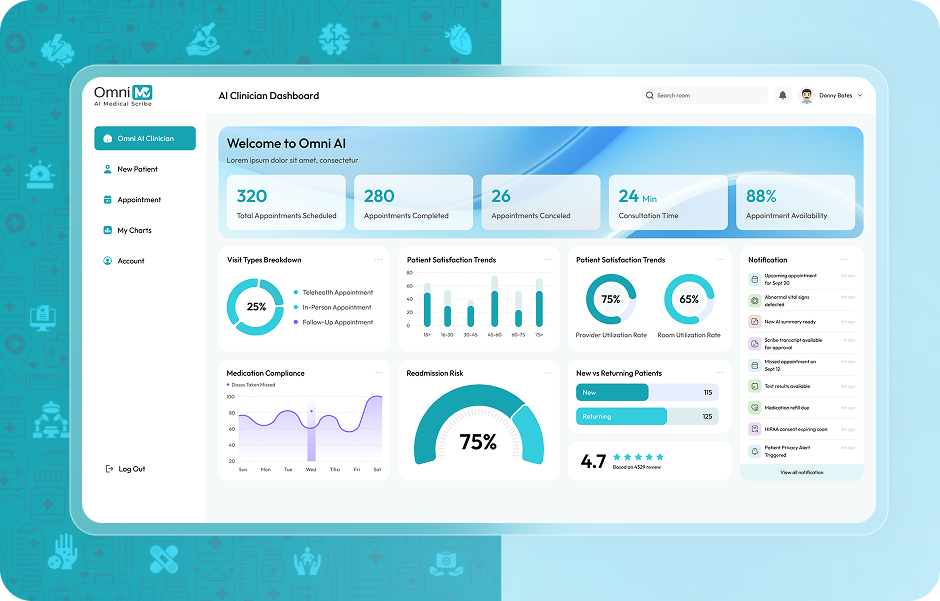
More Than Just An AI Scribe for Mental Health
Our behavioral health AI scribe does more than transcription. Built to function like an AI clinician partner, it supports assessment logic, DSM-aligned documentation, and treatment planning.
Save 15,000+ Hours in Mental Health Documentation
You hold complex stories every day, and your notes should honor that depth without draining your energy. OmnimD AI Scribe is especially designed for psychotherapy and psychiatry sessions, capturing mental status findings, risk assessments, medication updates, and treatment plan adjustments directly within your behavioral health EHR.
You can compare prior session narratives, track symptom evolution across visits, and view lab results or prescription history in one continuous chart. SOAP, DAP, and BIRP notes are structured around the language you actually use in therapy.
Progress toward goals remains visible at a glance, supporting clearer clinical decisions. Your focus stays on therapeutic presence while documentation aligns seamlessly behind the scenes.

Experience the Artificial Intelligence Scribe in Psychiatry
Psychiatric Note Automation
Automatically generates DSM-5–aligned psychiatric notes, including MSE, SOAP/DAP formats, risk assessments, and treatment plans. Reduces clinician burnout while maintaining compliance and structured behavioral health documentation standards.

Therapy Session Transcription
Converts therapy sessions into clinically structured notes using NLP trained on behavioral health terminology like CBT, trauma therapy, and medication management. Enables real-time documentation without disrupting therapeutic engagement.
Behavioral Health EHR Sync
Seamlessly syncs with behavioral health EHRs to auto-populate ICD-10 diagnoses, CPT codes (e.g., 90837, 90792), and outcome measures like PHQ-9 and GAD-7. Ensures billing accuracy, audit readiness, and continuity of care.
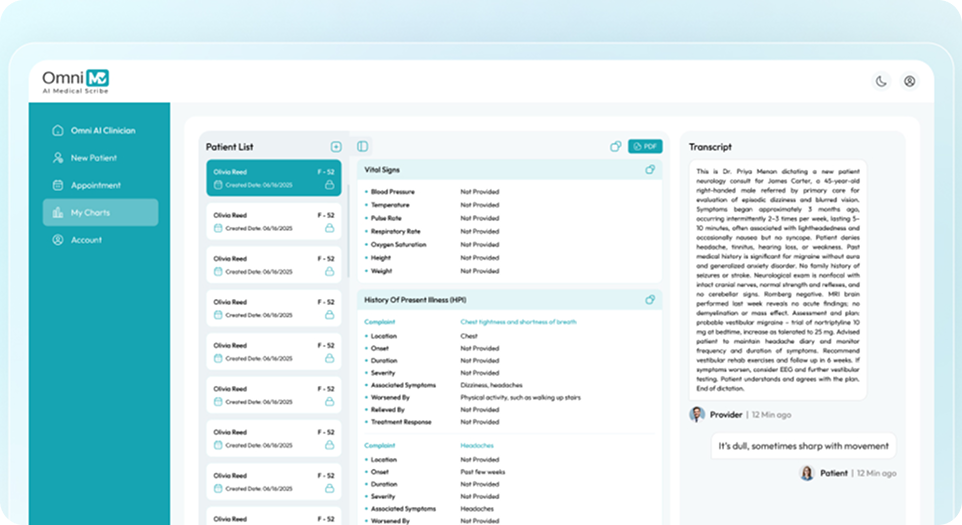
Clinician-Patient Voice Separation
Uses AI-based voice separation to distinguish clinician and patient speech during therapy sessions. Maintains narrative clarity and accurate attribution of clinical observations and patient statements.
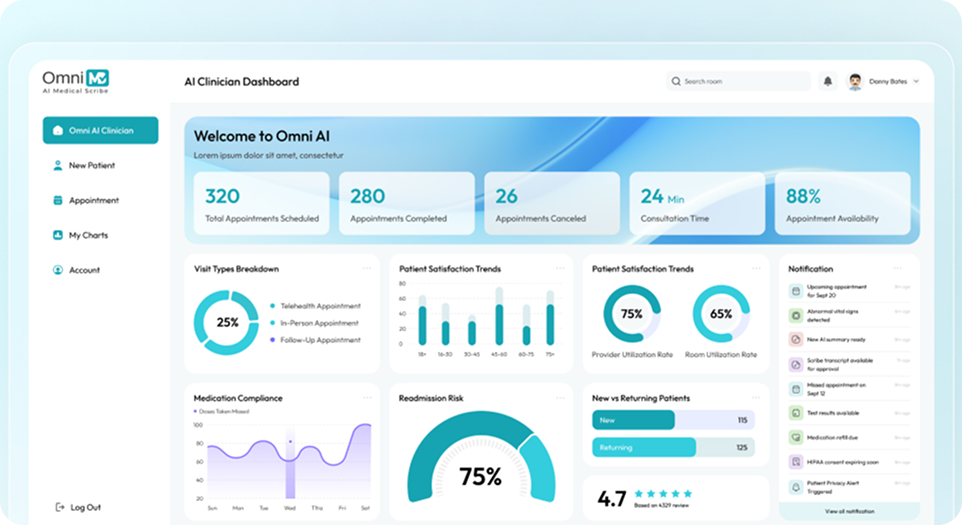
Multilingual Mental Health Processing
Processes multilingual therapy conversations while preserving contextual understanding of emotional and diagnostic language. Supports culturally sensitive documentation for diverse patient populations.
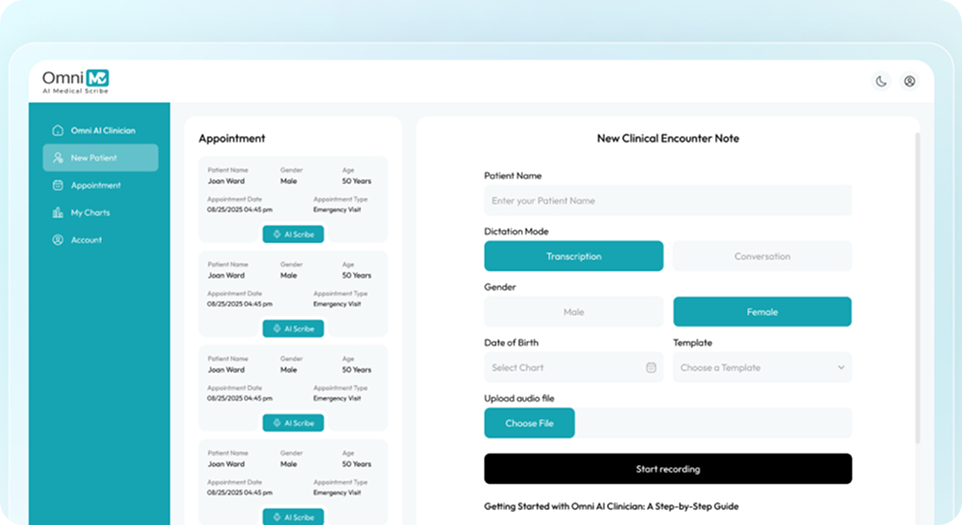
Session Summary Generator
Generates concise clinical summaries highlighting symptom trends, treatment response, and risk factors across sessions. Supports measurement-based care and faster clinical decision-making.
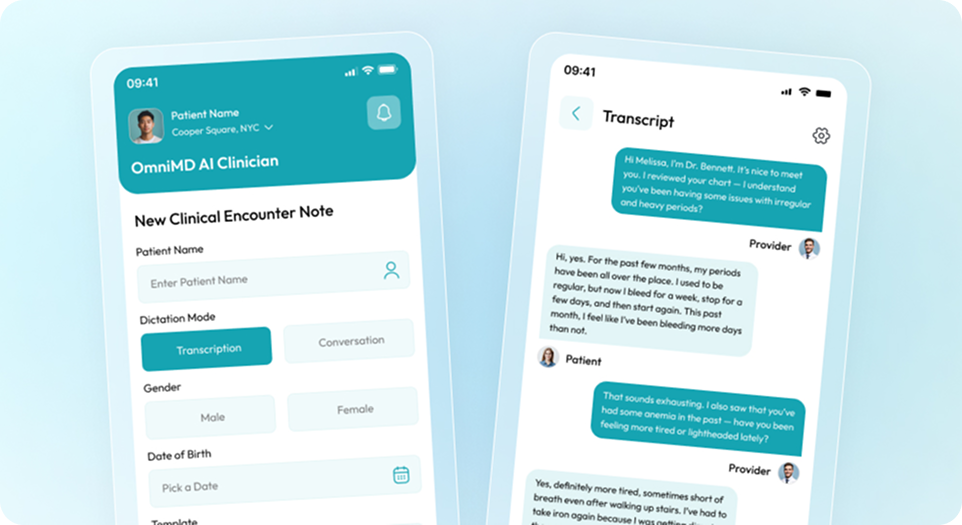
Longitudinal Record Comparison
Compares current and past mental health records to detect symptom progression, medication response, and documentation gaps. Strengthens longitudinal tracking and compliance oversight.
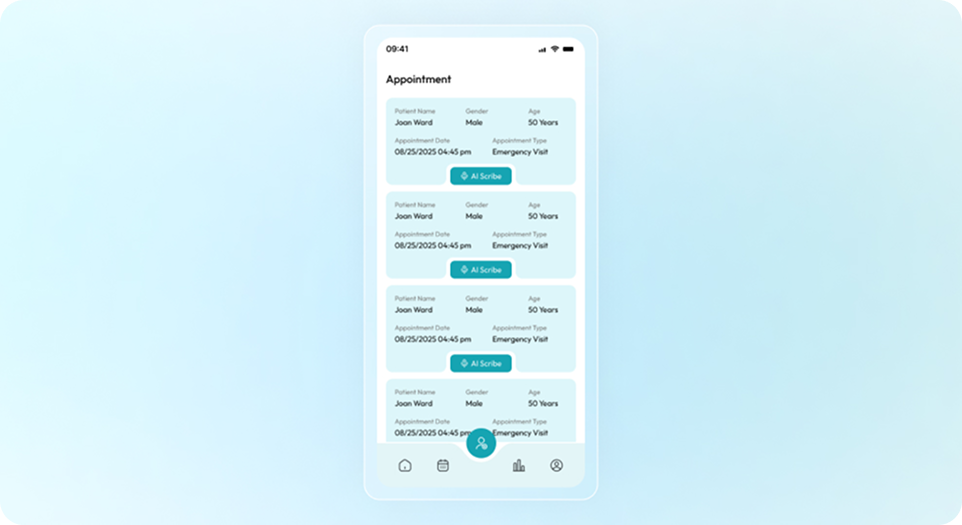
Exceeding Your Expectations