Epic vs NextGen: Get Answers to The Questions You’re Too Nervous to Ask
Let’s skip the intro about how the healthcare IT market is growing and get to what you actually need. You’re probably evaluating Epic EHR or NextGen Healthcare right now, you’ve heard horror stories about bad implementations, you’re worried about spending a lot of money on the wrong thing, and you want someone to just tell you the truth. That’s what this guide does.
Friction Point #1: “Am I even the right size for either of these?”
This is the question most people are too embarrassed to ask a sales rep directly. Here is the honest answer.
Epic
Epic was designed for organizations that have IT departments, implementation budgets in the millions, and clinical workflows that span inpatient, outpatient, surgical, pharmacy, and everything in between. It now covers 42% of all U.S. acute care hospitals and 55% of hospital beds.
If you run a solo practice or a 5-provider clinic, Epic is probably not the right fit. Not because it does not work, but because you would be paying for an enormous amount of capability you will never use.
NextGen
NextGen is different. It serves as healthcare technology partner for more than 8,000 organizations nationwide, representing 100,000 providers across 30 specialties and has genuinely strong workflows for practices from 1 to 100+ providers. But its sweet spot is mid-size specialty and behavioral health organizations. Very small practices sometimes find that even NextGen’s pricing is more than they need to spend.
Epic is right for you if you…
- Run a hospital, IDN, or academic medical center
- Have a dedicated IT team (or budget to build one)
- Need inpatient, outpatient, surgical, pharmacy all in one
- Have an implementation budget of $500K or more
- Are joining a health system on Community Connect
NextGen is right for you if you…
- Run an ambulatory EHR practice or specialty clinic
- Need deep specialty templates (30+ specialty types)
- Want 6 to 18 month ROI payback
- Are a behavioral health org or FQHC
- Want to be live in weeks, not years
Friction Point #2: “What does implementation actually feel like?”
Nobody in a vendor demo will tell you this. So we will.
One veteran CMIO described an EHR implementation as “probably the most disruptive psychosocial thing you can do to a clinician, outside of residency training.” That is not hyperbole.
Research published in JAMIA estimates up to 50% of EHR projects experience significant scope, budget, or outcome failures. The go-live period is where most of the damage happens.
A study published in theNational Library of Medicine highlighted that Epic’s implementation impacted communication and teamwork, workflow and efficiency, and patient care in the initial stages. The timeline for a hospital implementation runs 18 to 36 months from planning to go-live. Enterprise health systems can take even longer.
NextGen’s implementation is significantly faster.
Small practices can go live in weeks. A 20-provider specialty group typically takes two to four months. The productivity dip is still real, but shorter and shallower.
Real-world example
Intermountain Health consolidated different EHR systems across 33 hospitals into a single Epic instance. A few months post go-live, the system stabilized, and performance improved. But it took a full Epic migration to get there. That is a meaningful commitment in people, time, and cost that only makes sense at that scale.
Friction Point #3: “Will my staff burn out trying to learn this thing?”
This is one of the most underestimated risks in EHR purchasing decisions.
Physician burnout is at record highs, and the EHR is consistently identified as a contributing factor.
Choosing a system that is not well-matched to your workflows actively makes this worse.
Epic’s learning curve is steep. The system is powerful precisely because it is complex, and that complexity is real for frontline staff.
Industry best practices recommend substantial hands-on EHR training per clinical role, and cutting that to save money is one of the most documented predictors of implementation failure.
Epic’s Haiku and Canto mobile apps and the 2025 ambient AI integrations do genuinely reduce documentation burden once staff are trained. Getting there is the hard part.
NextGen users on G2 rate it 3.7 out of 5, with common complaints around system lag and customization difficulty. The specialty templates reduce the cognitive burden of documentation significantly for ambulatory providers, but ongoing support frustrations persist across mid-market EHR vendors.
That affects staff morale more than the software itself.
Epic’s customer support reality
Steep but survivable learning curve. Ambient AI via Art and Dragon Copilot meaningfully reduces documentation time post-training. Ask for serious training time. Do not skimp on at-the-elbow support during go-live.
NextGen client support reality
Ambient Assist saves 2.5 hours per day per provider once adopted. Support responsiveness is the most common frustration. Ask about dedicated account management before signing.
Friction Point #4: “Is the AI stuff real or just marketing hype?”
Both healthcare IT companies have real AI features in production today.
Neither is purely hype. The difference is depth and scale.
Epic’s AI is genuinely differentiated by data.
Its Cosmos database holds 300 million patients and 115 billion clinical events. No competitor trains on anything close to that. Its Art assistant handles ambient clinical documentation, diagnostics, and patient summaries. Penny generates medical coding suggestions and denial appeal letters automatically.
Mayo Clinic reported Art saves nurses 30 seconds per patient message while improving empathy. Epic’s Launchpad program in 2025 is accelerating deployment across its customer base. These are production results, not demo numbers.
NextGen’s Ambient Assist generates a full SOAP note in under 60 seconds at 90%+ accuracy. Specialty-specific models including ophthalmology launched in October 2024.
The Nia orchestrator (November 2025) is newer and ambitious, using voice commands to coordinate clinical, financial, and operational tasks. Ask to see it live in a demo before taking the claims at face value, it is genuinely new territory.
What neither AI does: it does not replace clinical judgment, it does not eliminate the need for training, and it does not work well if your practice’s data hygiene is poor going in.
Pain Point #5: “What am I actually going to pay? Be honest.”
Neither vendor will give you a number before a demo. Here is what independent sources, health system disclosures, and industry analyses show.
Epic: what you’re actually signing up for
Hospital implementation: $10M to $30M for a community hospital
Large system: $50M to $200M+ and up
10-provider ambulatory, 5yr TCO: $1.5M to $3M+
Per provider/month: $200 to $500
Go-live timeline: 6 months to 3 yearsROI payback: 3 to 7 years typically
NextGen: what you’re actually signing up for
Small practice setup: $50K to $150K
Larger enterprise: up to $500K
10-provider ambulatory, 5yr TCO: $250K to $700K
Per provider/month: $299 to $700
Go-live: weeks to a few months
ROI payback: 6 to 18 months typically
The hidden cost
Epic requires 2 to 5 certified IT FTEs post go-live, running $150K to $500K per year in salaries. NextGen’s base subscription routinely excludes population health management, advanced analytics, and managed RCM.
Always get a fully scoped all-in quote. The sticker price is never the real price.
Trinity Health projected $1 billion in ROI from Epic across 92 hospitals over 10 years. That math only works at 92 hospitals. At 10 providers, you are looking at a very different equation entirely.
So what do you do if you just did that math and realized neither option really fits your size or budget?
Scroll down.
We are about to show you something most comparison guides never mention.
The third option that you were missing out on
Most practices comparing Epic vs NextGen Healthcare are unconsciously assuming those are the only two real options. They are not. There is a platform that has been serving independent and mid-size practices for over 20 years, quietly delivering the features that matter without the enterprise price tag. It is called OmniMD.
Here is why it deserves serious consideration, with everything sourced so you can verify it yourself.
- It is fully certified and genuinely integrated. ONC-certified, AI-powered, with 18+ products covering EHR software, practice management software, revenue cycle management, telehealth, and remote patient monitoring under one login. You are not piecing together five vendors.
- The AI documentation is native, not a third-party bolt-on. Real-time ambient listening, SOAP note generation, and ICD-10 and CPT auto-coding are all built in-house. When something breaks, there is one call to make. That matters a lot at 2am.
- The billing numbers hold up. 90% clean claim rate and average A/R reduced to 29 days. That is comparable to what NextGen’s managed RCM delivers at a fraction of the cost.
- It serves 12,000+ healthcare professionals across 600+ U.S. facilities across 20+ specialties including cardiology, psychiatry, pediatrics, and urgent care. These are not pilot users. They are long-term customers.
- Go live in days, not months. Capterra and Software Finder reviews consistently praise fast implementation and responsive support, both of which are areas where NextGen has drawn criticism.
- 5-year TCO is meaningfully lower. Pricing starts around $500 to $1,000 per month for the practice, putting the 5-year TCO at roughly $150K to $400K versus NextGen’s $250K to $700K for a comparable-sized practice.
If you are a practice with 1 to 30 providers and you have spent the last few weeks comparing Epic and NextGen thinking those are your only two options, you may be about to make a significantly more expensive decision than you need to. Book a demo. Spend an hour. It could save you hundreds of thousands of dollars.
Friction Point #6: “Will it actually talk to my labs, pharmacy, and payers?”
KLAS rated both Epic and NextGen 4.25 out of 5 on EHR interoperability, the highest tier. On paper they are equal. In practice, scale matters.
- Epic exchanges 20 million patient records every day through Care Everywhere. Its FHIR API library has 700+ open specs and 1,000+ third-party apps. It became a TEFCA QHIN in December 2023 and had 1,000+ hospitals connected by mid-2025. Lab, pharmacy, imaging, and payer connections at the hospital level are comprehensive and well-tested.
- NextGen achieved HTI-1 compliance ahead of the December 2025 federal deadline. Its Mirth Connect integration engine powers one-third of all U.S. public HIEs and is used in 40+ countries. A Kno2 TEFCA partnership launched September 2025 connecting 100,000+ providers. For ambulatory practices, this is more than sufficient.
Friction Point #7: “What if the vendor relationship turns sour, or they get sold?”
This is a legitimate fear and most buyers do not ask about it directly enough.
Epic is about as stable as a private software company can be. $5.7 billion in 2024 revenue, employee-owned, and founder Judy Faulkner has publicly rejected acquisition offers including a reported $30 billion bid. The product direction score on G2 is 4.2 out of 5. Customers believe in the roadmap. The main concern with Epic is not instability, it is cost lock-in once you are deep into a multi-year enterprise deployment.
NextGen is a different story. Thoma Bravo acquired it for $1.8 billion in November 2023, then Madison Dearborn Partners co-invested in June 2025. Private equity in healthcare IT typically operates on a 5 to 7 year exit horizon, which means a sale, merger, or IPO is likely before 2030.
That is not necessarily bad for you as a customer, but it does mean pricing, product focus, and support models could change. Get explicit contractual protections on pricing and service levels before you sign a multi-year deal.
Friction Point #8: “What happens when something breaks at 2am?”
Support quality is where the gap between these two vendors is most felt day-to-day.
The feature list matters less than what happens when you have a billing problem the night before payroll.
Epic’s support model relies heavily on your organization’s internal Epic-certified staff and, for escalations, Epic’s own support channels. G2 rates Epic’s quality of support at 4.2 out of 5.. For large health systems with dedicated Epic teams, this works well. Smaller organizations on Epic often feel exposed if they do not have enough certified staff in-house.
NextGen’s support has historically been a pain point for some customers, though the picture is more nuanced than it once was. In the 2026 Best in KLAS report, NextGen Healthcare was actually recognized for significant year-over-year score improvement, one of several vendors singled out for meaningful gains. That said, relationship quality and support responsiveness are still areas worth scrutinizing, particularly for practices without in-house IT staff who depend on the vendor to resolve issues quickly. Ask specifically about dedicated account management, escalation pathways, and typical ticket resolution times before you commit, and if possible, talk to reference customers of similar size about their day-to-day support experience.
Pick your path: the decision flowchart
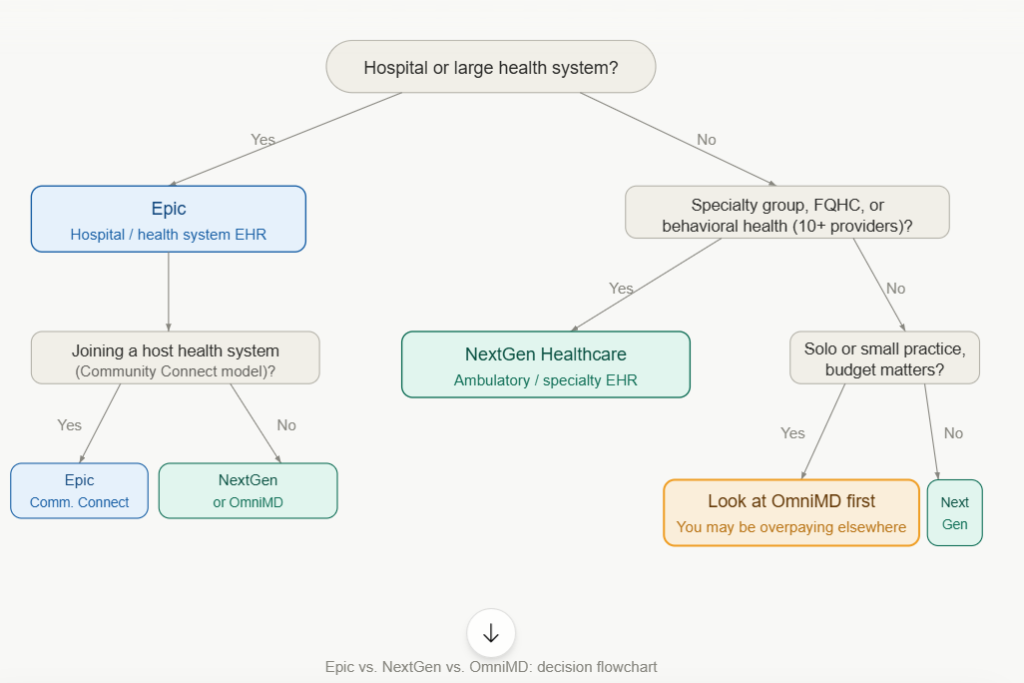
Before you book your first vendor demo, do this
If Epic is on your list
- Check Epic Community Connect availability through a local host health system before going direct. The cost difference can be 5x. Read the governance terms about data ownership and operational control carefully.
- Ask for a 5-year total cost of ownership projection that includes IT staffing, hardware refresh, training, and the go-live productivity dip. Those hidden costs routinely exceed the software contract value.
- Ask specifically which AI features (Art, Emmie, Penny) are base contract versus separately licensed add-ons. AI pricing is changing monthly right now.
- Find references from organizations that went live in the last 18 months. Use CHIME or AHA networks, not the vendor’s suggested contacts. Ask them specifically about support quality during and after go-live.
If NextGen is on your list
- Demand a fully scoped quote that includes population health management, analytics, and managed RCM. The base subscription routinely excludes all three. You need the all-in number before any meaningful comparison.
- Run a 30-day Ambient Assist pilot with your actual providers before signing anything. Ambient AI accuracy varies by specialty. Validate it in your real workflows, not a curated demo.
- Verify Mirth Connect licensing terms for every integration you need. The shift to proprietary licensing in version 4.6 has implications for organizations that built on the free community version.
If OmniMD is on your radar
- Ask about the free EHR offer with their billing contract. If you currently outsource billing, this conversation alone could be worth tens of thousands of dollars.
- Request a live demo of the ambient listening and auto-coding workflow in your specific specialty. It is built natively. One vendor, one support call when something breaks.
Ask for a walkthrough of specialty-specific reporting and analytics for your area. Know exactly what you are getting before you compare it to NextGen’s offering.