Your Denied Claims Are Still Worth Fighting For and Our Denial Management Experts Know Exactly How
Insurance denials are the opening move in a process most practices don’t have the dedicated bandwidth to see through. Our specialist takes over exactly where your billing staff has to stop, and we stay with every denied claim through investigation, appeal, and resolution.
4 Compounding Reasons Your Medical Billing Denial Rate Keep Draining Your AR

01
Deadlines slipping through
Every denied claim comes with an appeal window, and once that window closes, your right to contest the decision closes with it. When nobody is actively tracking appeal deadlines across every payer and every claim, that window expires by default, and recoverable revenue goes with it.

02
The same root causes repeating
When there is no systematic denial tracking and root cause reporting in place, nothing upstream ever gets corrected. The same eligibility gaps, coding mismatches, and documentation oversights keep generating the same denials, costing your practice in lost revenue and in the time spent dealing with issues that were entirely preventable.

03
Underpayments absorbed without question
Insurance payers routinely reimburse below contracted rates, and without line-level payment variance analysis against your fee schedule, those underpayments get posted and accepted as though they were accurate. The shortfall reduces what your practice collects over time, and it rarely shows up anywhere obvious.

04
Appeals built without payer-specific knowledge
UnitedHealthcare, Aetna, BCBS, Cigna, and every regional carrier all have their own documentation standards, reviewer criteria, and escalation paths. An appeal that doesn’t address what that specific payer requires to reverse a denial has very little chance of succeeding, regardless of how strong the underlying case actually is.
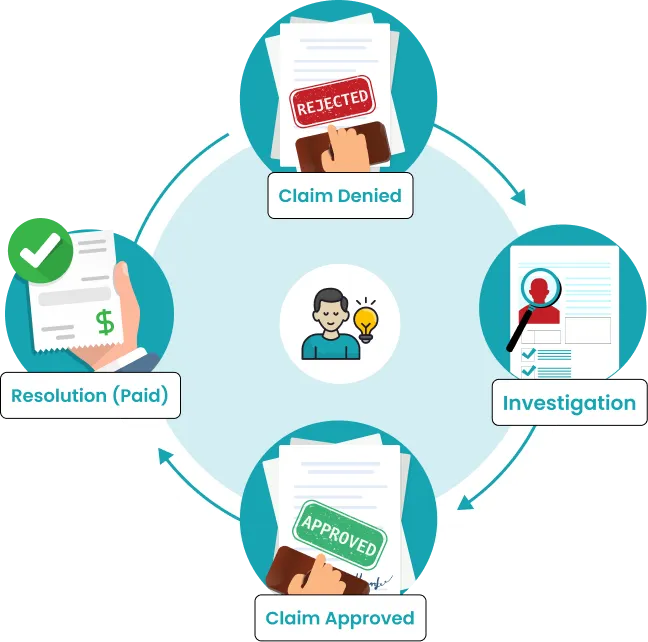
Everything That Happens After a Medical Claim Denial, That’s Where We Step In
We take over the denied and underpaid portion of your AR entirely, investigating what actually caused each denial, building an appeal tailored to the specific payer’s review standards, filing through the right channel, and tracking every open case through to final resolution.
Denial triage and deadline mapping
Every denied claim is logged by payer, denial reason code, billed amount, and appeal deadline the moment it arrives. Priority is set by urgency, because a missed deadline on any claim is revenue that cannot be recovered regardless of how strong the appeal would have been.
Payer-specific appeal construction
Every appeal is built around how that specific payer’s reviewers actually evaluate disputes, what clinical documentation they need, what authorization records they want to see, and how the argument needs to be framed to move. That level of specificity is what separates appeals that get reversed from appeals that get filed and forgotten.
Underpaid claim recovery
We run payment variance audits against your contracted fee schedule as a standard part of every engagement. When a payer has reimbursed below agreement, we dispute it formally with full documentation and follow it through to resolution.
AR denial management and follow-up
A claim does not close in our system until it has been fully resolved, paid at the correct amount, adjusted for a legitimate contractual reason, or genuinely exhausted through every available appeal channel.
Denial tracking and reporting
Every month you receive a report showing exactly which payers are generating the most denials, what reason codes are driving them, and what specific changes your team can make upstream to reduce the volume coming back in the first place.
Here’s What Revenue Recovery From Denied Claims Looks Like Across the Practices We Work With
94%
First-pass appeal success rate across all payers and specialties
21 Days
Average time from claim intake to final resolution
3.2x
Average return practices see on our engagement fee
Under 2%
Average denial rate for clients after six months
Who Our Denial Management Services Are Built For

Physician and group practices
High-volume commercial payer denials across complex E&M, surgical, and diagnostic claims require payer-specific knowledge that most in-house billing teams don’t have the capacity to develop. We bring that depth to every claim we work.

Behavioral health providers
Behavioral and mental health specialties carry a disproportionate share of medical necessity denials and coverage limitation disputes. We build the clinical justification documentation these appeals require to actually move a payer reviewer.
Outpatient surgical centers
High-dollar procedures make the stakes of getting an appeal right considerably higher. We handle authorization-related denials and procedure-specific appeal documentation for ASCs across a wide range of specialties.

Practices with in-house billing teams
Your team handles claim submissions and we handle everything that comes back refused. We work the denied AR your billing staff does not have the bandwidth to pursue without pulling them away from keeping your revenue cycle moving forward.
What Sets Our Claim Denial Resolution Apart
Payer intelligence applied directly
We maintain current working knowledge of how UnitedHealthcare, Aetna, BCBS, Cigna, and regional carriers across the country actually review and respond to appeals, and every appeal we build reflects that knowledge directly.
Underpaid claim recovery always in scope
Payment variance audits against your contracted fee schedule are a standard part of every engagement, and if a payer has paid below your contracted rate, we treat it the same way we treat any other denial: something to be formally addressed and recovered.
A model built around your results
We earn on outcomes, you retain the substantial majority of everything we recover, and there is no long-term lock-in beyond the value we are actively delivering.
Know Where Your Practice Stands
Get better visibility into your workflows and readiness for performance-based care – before it impacts your reimbursement.