Top EHR/EMR Integration Companies & What They Actually Do
EHR integration simply means connecting an EHR (or EMR) system with another piece of software, app, or device so that they can share patient data with each other. This sounds easy, but it is not because:
- Every hospital and clinic uses a different EHR brand, and there are hundreds of them on the market.
- Each EHR stores data in its own way, in its own format, with its own rules.
- Patient data is highly sensitive, so every connection has to be secure, legal, and audit ready.
- Hospitals are slow to approve new connections because they do not want to risk patient safety or compliance fines.
This is why so many companies have built their entire business around solving this one problem. The tools they offer are usually called EHR integration services or healthcare data integration platforms. But here is the catch. Every vendor on this list is good at something different. The real question is not which one is “best.” It is which one fits the practice or product you are running, and when you should choose that one over the others. That is the question this post is built to answer.
Why Is This Such a Big Deal Right Now
There are four main reasons EHR integration has become one of the hottest topics in healthcare technology in 2026.
1. The EHR market is split across many vendors.
In the US, Epic alone holds roughly 37.7 percent of the acute care hospital market and 43.92 percent of the ambulatory (outpatient) market. After Epic, you have Oracle Health (the new name for Cerner), Veradigm (formerly Allscripts), athenahealth, eClinicalWorks, MEDITECH, NextGen, and many smaller players. If you are building a digital health product or running a multi state practice group, you cannot just pick one EHR and call it a day. You need to connect to several. That is exactly what EHR integration companies help you do.
2. The government is forcing the issue.
A wave of federal rules is pushing every healthcare organization toward open, standard data sharing. The 21st Century Cures Act bans information blocking. The ONC HTI-1 Final Rule mandates support for the US Core Data for Interoperability (USCDI) through FHIR APIs. The CMS-0057 rule requires FHIR based prior authorization workflows. And TEFCA (the Trusted Exchange Framework and Common Agreement) is creating a nationwide network of health information exchanges. All of this is pulling data out of silos and into shared, standardized formats, and almost no in-house team can keep up alone.
3. The market is growing fast and the dollars prove it.
The healthcare interoperability market was valued at around 6.68 billion dollars in 2025 and is projected to grow past 16 billion dollars by 2034. The healthcare data integration platforms market is growing at a double digit rate, with North America holding about 42 percent of global share. Companies like Microsoft, Oracle Health, Redox, and InterSystems are all racing to grab their piece. According to a 2024 Accenture survey, more than 85 percent of healthcare CIOs plan to increase spending on interoperability over the next 12 months.
4. Patients and clinicians are tired of the old way.
Nobody wants to fill out the same paper form three times in one visit. Nobody wants to wait two weeks for records to be faxed (yes, faxed) from one hospital to another. And clinicians are burned out from clicking between five different systems just to see one patient’s full picture. A KLAS Research survey called EHR Interoperability 2024 found that only 44 percent of clinicians felt their EHR gave them the level of external integration they expected. That gap is exactly what these integration companies are trying to close.
Where HL7 and FHIR Fit In
Two terms come up over and over in this space. You will see them on every integration company’s website, and they will shape what you can and cannot do with each vendor.
HL7 stands for Health Level Seven. It is the older messaging standard that most hospital systems still use to send things like admissions, lab orders, lab results, and billing data between systems. HL7 v2 has been around for decades and is reliable, but it is also clunky and not built for modern web apps. HL7 integration is still the workhorse for most real time hospital workflows.
FHIR stands for Fast Healthcare Interoperability Resources. It is a newer standard, also created by HL7 the organization, that uses modern web technology like REST APIs and JSON. FHIR is what powers most patient apps, mobile health tools, and AI products today. FHIR integration is where the industry is heading, and government rules now require it for things like patient access and prior authorization.
In real life, healthcare organizations almost always need both HL7 and FHIR support. HL7 keeps the lights on, and FHIR powers the new stuff. Any integration company worth considering has to handle both.
Now let’s get into the companies that actually do this work, what your practice or product gets from each one, and when each is the right call.
1. Redox
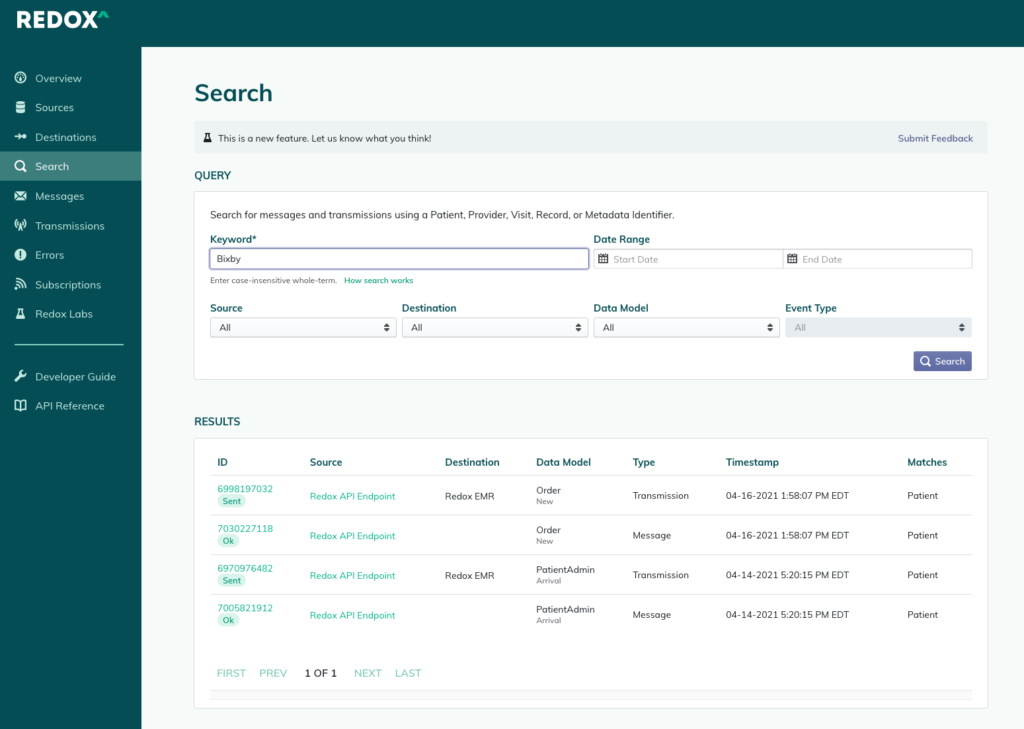
If you ask anyone in digital health about EHR integration, Redox is often one of the first names you’ll hear. That’s not accidental. They’ve positioned themselves as a broad, horizontal integration layer for healthcare, and they are arguably the most recognized name in the category.
What you get with Redox
At a practical level, Redox acts as a middle layer between your product and multiple EHR systems.
Instead of building and maintaining separate integrations for systems like Epic, Oracle Health (Cerner), athenahealth, or Meditech, you build once to Redox. Redox then manages the downstream connections.
You also get format translation out of the box. Healthcare data often comes in older standards like HL7 v2, CDA, X12, or DICOM. Redox converts that into more modern formats like JSON or FHIR so your engineering team can work with cleaner, more usable data.
In short, what you get is reach without the engineering tax. You stop building one-off pipes to every hospital and start managing one connection that fans out to many.
What stands out
Redox is strongest when you need scale. If your product needs to connect to many health systems or EHRs at once, this model reduces the number of integrations you need to manage directly.
Their platform also removes a lot of infrastructure burden. Many teams use Redox to avoid managing VPNs, interface engines, and custom parsers for legacy formats.
What to expect on pricing
Redox does not publish pricing publicly, but their structure is fairly typical for middleware:
- A platform fee based on scope and support level
- A volume-based component tied to message or transaction count
- Professional services for custom work
For early-stage companies, Redox has indicated that discounts may be available, but this is something you need to confirm during evaluation.
Implementation reality
Redox is often faster than building integrations yourself, but it is not instant.
If an EHR connection already exists in their network, timelines can be relatively short. But every hospital or health system still needs to approve access, complete security reviews, and configure workflows. That part does not disappear.
Customer feedback generally highlights faster onboarding compared to building from scratch, but also notes that custom data mapping or non-standard fields can require additional work with Redox’s team.
What’s changed recently
One of the more important developments is Redox’s partnership with Kno2, a Qualified Health Information Network under TEFCA. This matters because it brings nationwide data exchange capabilities more directly into their platform.
When you should choose Redox
Choose Redox when:
- You are a digital health vendor, and your product needs to plug into many EHRs across many hospital systems.
- You are a payer or enterprise platform that needs broad interoperability without spinning up an integrations team for every customer.
- You value speed of reach over deep customization, and you would rather standardize on one middleware than maintain custom code for every connection.
This is the right choice when your problem is breadth. The more EHRs you need to touch, the more sense Redox makes.
What to keep in mind
Redox simplifies integration, but it does not eliminate the operational work. You still need to handle workflows, data mapping decisions, and coordination with each healthcare organization.
2. Vim
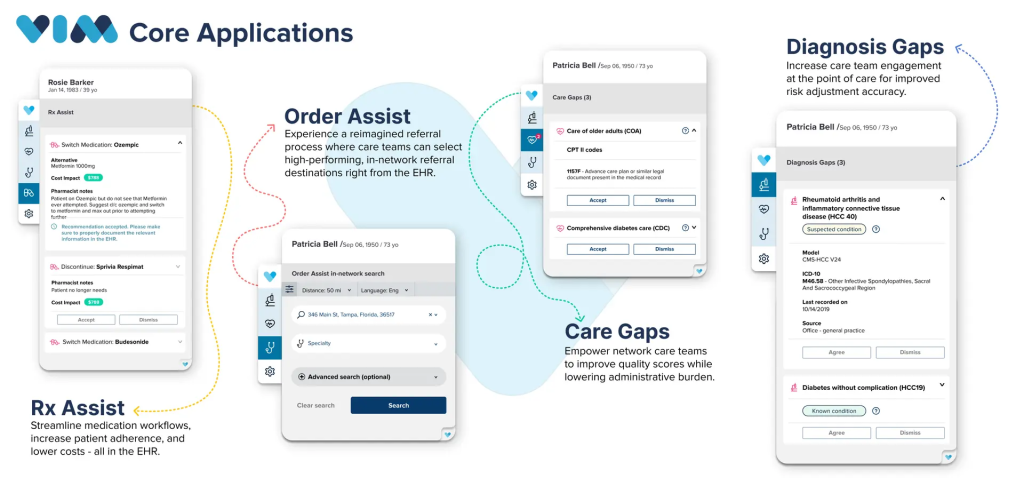
Vim earns its place on this list by approaching integration from a different angle. Instead of focusing primarily on moving data between systems, it focuses on where that data shows up. That makes it the right pick for a very different kind of buyer than Redox.
What you get with Vim
Vim embeds applications and data directly inside your EHR interface.
In practice, this means clinicians do not have to leave their workflow to access external tools. Information, alerts, or actions appear inside the EHR they are already using.
Their platform has two main components:
- Vim Connect, which integrates into the EHR interface
- Vim Canvas, which provides APIs, SDKs, and a developer platform
What you get, in plain terms, is influence at the point of care. Care gaps, risk codes, and recommendations show up where the clinician is already working, not in a separate dashboard nobody opens.
Why this matters
Most integration platforms focus on data access. Vim focuses on workflow.
This becomes especially important in value-based care, where the goal is not just to access data, but to influence decisions at the point of care.
Vim supports both reading from and writing back to the EHR, with user authorization. That enables actions like updating diagnoses, adding procedure codes, or closing care gaps directly within the workflow.
Implementation expectations
The company positions itself as relatively fast to deploy from a development perspective. Their SDK is designed to support quick application builds.
However, like any EHR-connected solution, actual rollout timelines depend on provider adoption, approvals, and configuration inside the healthcare organization.
Things you should verify
Unlike some competitors, Vim does not prominently publish detailed security certification pages. That does not mean they lack them, but it does mean you should explicitly ask:
- Which certifications are current
- When audits were last completed
- Whether reports can be shared under NDA
There is also a technical constraint worth noting. Vim requires your application server to be hosted in the United States for production use.
Recent developments
Vim has been expanding its ecosystem through partnerships and by building out its developer platform. There has been a noticeable push toward embedding AI-driven insights, especially in areas like risk adjustment and care gap identification.
When you should choose Vim
Choose Vim when:
- You are a value-based care organization, and your success depends on actually changing clinician behavior, not just reporting on it.
- You are a health plan, and you need risk adjustment, care gap closure, or prior authorization actions to happen during the visit, not after.
- You are building a clinical tool that needs to live inside the EHR screen because clinicians will not log into a second system to use it.
This is the right choice when your problem is adoption at the point of care. If your data is already moving but nobody is acting on it, Vim is the layer that fixes that.
What to keep in mind
Vim is not a direct replacement for platforms like Redox. Many organizations use both.
Redox handles large-scale data movement. Vim focuses on how that data shows up and gets used in clinical workflows. If you need both reach and in-workflow influence, you may need both.
3. Medbridge
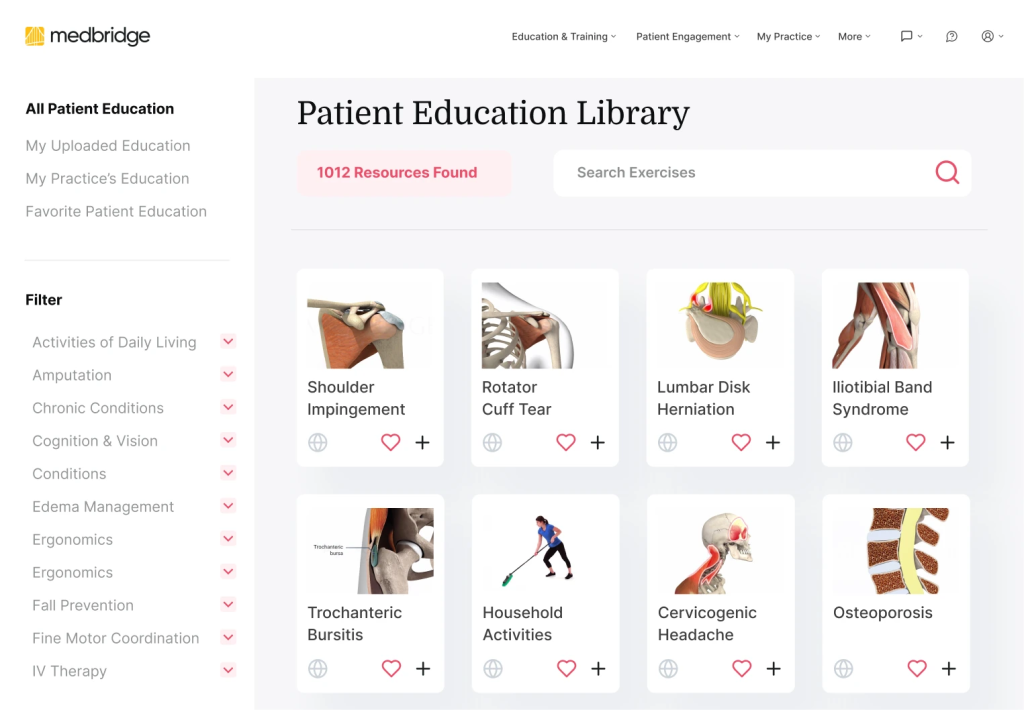
Medbridge is often misunderstood in conversations about integration. It is not primarily an integration company. But it earns a spot on this list because of what it delivers to a very specific kind of practice, rehab teams that want clinical content and patient engagement showing up directly inside the EHR they already use.
What you get with Medbridge
Medbridge gives a rehab practice four things in one bundle:
- Continuing education for clinicians
- Home exercise programs
- Patient engagement tools and remote therapeutic monitoring
- Digital triage capabilities
Their integrations allow clinicians to access and use these tools directly within their EHR, particularly in rehab-focused workflows. So rather than buying a content library, a HEP tool, and a patient engagement app separately and then trying to glue them together, you get them already wired into the systems your therapists work in.
Integration scope
Medbridge has direct integrations with several systems, including Epic, NetHealth, and NextGen. For broader connectivity, they rely on middleware platforms like Redox.
This hybrid approach is fairly common for companies that are not primarily integration vendors but still need to show up inside many different EHRs.
Implementation reality
For Epic integrations, Medbridge typically cites timelines in the range of a few months. Required technical effort on the client side is relatively limited compared to building custom integrations.
Pricing clarity
Medbridge does publish some pricing for individual plans, particularly for education-focused offerings. However, enterprise or integration-heavy deployments are usually custom priced.
Third-party pricing directories can give rough estimates, but these should always be validated directly with the vendor.
Customer feedback
Users tend to highlight:
- Strong content libraries
- Ease of use
- Improved patient adherence through digital tools
Common complaints are more workflow-related, such as navigation friction or session timeouts, which are often tied to compliance requirements.
Vendor-reported outcomes
Medbridge publishes performance metrics like time savings and revenue impact. These should be treated as directional rather than guaranteed outcomes. It is always better to validate with reference customers in your specific specialty.
Recent developments
Medbridge has been investing in AI capabilities, particularly through motion capture and movement analysis. They are also expanding into virtual MSK care models through partnerships.
When you should choose Medbridge
Choose Medbridge when:
- You run a physical therapy, rehab, or MSK-focused practice and want education, HEPs, and patient engagement bundled in one tool.
- Your therapists already live inside Epic, NetHealth, or NextGen, and you want to avoid forcing them into a separate app.
- Your clinical priority is patient adherence and outcomes, not custom data pipelines.
This is the right choice when your problem is rehab workflow content, not generic data exchange. If you are not in the rehab world, the other vendors on this list will fit you better.
Important clarification
Medbridge the software company is not the same as MedBridge Healthcare, which is a separate organization in the respiratory and sleep therapy space.
4. Datavant
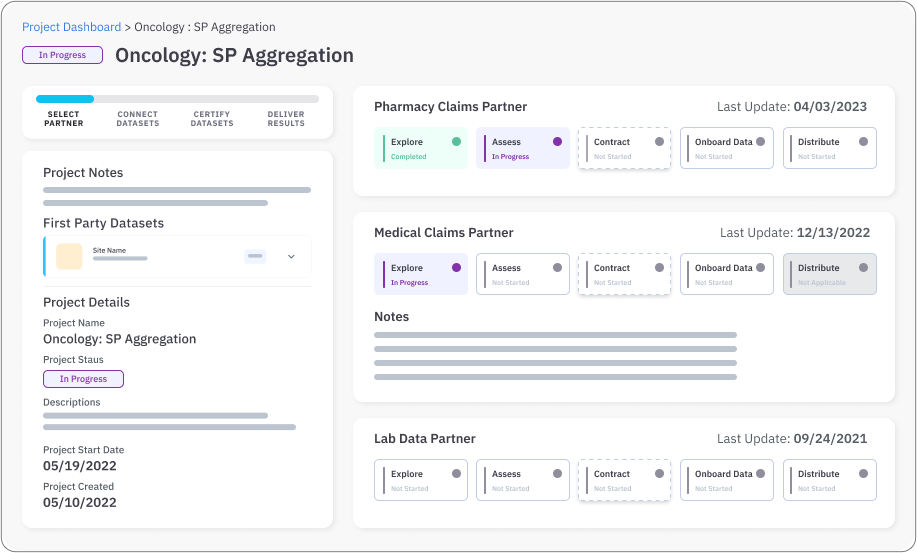
Datavant operates in a different category altogether. While others focus on real-time workflows, Datavant focuses on large-scale data movement and record retrieval. It is the right pick when the problem is volume and compliance, not instant access.
What you get with Datavant
Datavant gives you the heavy machinery for moving and connecting health records at scale. That includes:
- Medical record retrieval
- Release of information workflows
- Data tokenization and de-identification
- Real-world data for research
- Large-scale data linkage
They connect to a wide range of EHR systems through an interface engine, but their primary value is in handling volume and compliance.
What you get is not faster clinical screens. What you get is the ability to pull thousands of records for risk adjustment, link patient data across sources for research, or hand off de-identified data to a life sciences partner without compliance risk.
Where they fit
Datavant is particularly strong in use cases like:
- Risk adjustment
- HEDIS reporting
- Legal and insurance record retrieval
- Clinical research and real-world evidence
This is less about real-time clinician workflows and more about data logistics across the healthcare ecosystem.
Implementation expectations
Some components, like installing extraction tools, can be relatively quick. However, broader deployments, especially at the enterprise level, can take significantly longer.
Timelines vary widely depending on the use case.
Pricing model
Datavant’s pricing depends heavily on the product:
- Some patient-facing and requester tools are free
- Record retrieval may be priced per request
- Enterprise solutions are custom and volume-based
Pricing is also influenced by regulatory constraints around medical record fees, which vary by state.
Security posture
Datavant emphasizes compliance, including HIPAA, SOC 2 Type 2, and HITRUST certifications. They have also publicly discussed the scale of investment required to build their compliance infrastructure.
Recent developments
The acquisition of Ontellus expanded their presence in legal and insurance workflows. They have also achieved validation milestones that simplify data use in quality reporting.
When you should choose Datavant
Choose Datavant when:
- You are a health plan that needs to retrieve thousands of charts for risk adjustment or HEDIS, and your current process is manual, slow, or both.
- You are a life sciences organization that needs real-world data with proper de-identification and tokenization built in.
- You are a large health system or law firm dealing with high volume release-of-information requests and you cannot keep up with them.
This is the right choice when your problem is bulk records and compliance, not bedside data. Do not pick Datavant if you are trying to put information in front of a clinician during a visit.
What to keep in mind
Datavant is not designed for real-time EHR interactions. If your goal is to display data inside a clinician’s workflow instantly, you will likely need a different type of platform.
5. OmniMD
Up to this point, we’ve looked at companies that primarily focus on connecting systems. OmniMD belongs in this conversation for a different reason. We are not just an integration layer. We are a complete, AI-driven healthcare platform that includes a built-in EHR, the surrounding ecosystem, and the integration capabilities most practices actually need.
For a lot of independent practices and specialty clinics, the integration question is not “how do I connect ten different vendors?” It is “how do I get a system that already does most of this, and then connects cleanly to the few outside tools I really need?” That is the practice OmniMD is built for.
What you get with OmniMD
At OmniMD, we bring together multiple core functions into a single, connected platform:
- Electronic Health Records
- Practice Management
- Revenue Cycle Management
- Telehealth
- Remote Patient Monitoring
- Patient engagement tools
What you get is a working clinical, operational, and financial stack out of the box, with these components already designed to talk to each other. That cuts out a large chunk of the integration burden before it even starts. Instead of buying an EHR, then an RCM tool, then a telehealth platform, then trying to connect them, you get one system where the connections already exist.
How we approach external integration
Even as a full platform, integration still matters. Healthcare systems do not operate in isolation.
We support widely used interoperability standards such as HL7 and FHIR, along with custom API-based integrations. This allows us to connect with:
- Laboratories and diagnostic systems
- Imaging platforms using DICOM
- Third-party clinical and administrative tools
Our approach is to balance two things. First, reduce the number of integrations you need by offering more capabilities natively. Second, make external integrations easier and more flexible when they are required.
What to expect on pricing
Like most healthcare platforms, pricing is not one-size-fits-all.
Costs typically depend on:
- The modules you choose, such as EHR, RCM, telehealth, or AI tools
- The size and complexity of your organization
- Implementation, training, and support requirements
Some third-party directories provide estimated starting ranges, but these should be treated as directional only. The most reliable way to evaluate cost is through a detailed quote that includes all components of your deployment.
What customers consistently tell us
Across aggregated reviews and long-term client relationships, a few themes show up repeatedly:
- The platform is relatively easy for new staff to learn
- Specialty-specific templates align well with real clinical workflows
- Support teams are responsive, with many clients staying for years
There are also areas where we continue to improve:
- Certain workflows can require more steps than expected
- Some advanced customizations involve support team collaboration
- Specific features, like parts of e-prescribing workflows, can feel less simplified in high-volume environments
We take this feedback seriously because usability at the point of care directly impacts outcomes and efficiency.
What we’ve been building recently
A major focus for us over the past few years has been AI-driven functionality across the platform.
This includes:
- AI-powered ambient documentation to reduce manual charting
- AI-assisted front desk operations for scheduling and patient communication
- Clinical support tools that help with charting and insights
- Automation within billing and revenue cycle workflows
We have also expanded our lab integration capabilities, supporting smoother data flow between laboratory information systems and the EHR through HL7, FHIR, and APIs.
When you should choose OmniMD
Choose OmniMD when:
- You are an independent practice or multi-specialty clinic that wants one platform instead of stitching together five.
- You are tired of paying separate vendors for EHR, RCM, telehealth, and patient engagement, and you want them already connected.
- You want AI-driven documentation, scheduling, and billing built in, without buying it as a bolt-on from another vendor.
- You want lab, imaging, and third-party tool integrations through HL7, FHIR, and APIs, but you do not want to run a middleware platform yourself.
This is the right choice when your problem is the cost and complexity of running a stack of vendors. If you would rather solve integration by needing fewer integrations in the first place, this is the path.
What to keep in mind
Choosing an all-in-one platform is a different strategic decision compared to choosing a pure integration vendor.
With OmniMD, you are not just solving for connectivity. You are standardizing how your organization manages clinical, operational, and financial workflows, and reducing how many integration points you have to maintain in the first place.
For many practices, this reduces complexity over time. But it also means taking a more holistic approach to system adoption, rather than solving one integration use case at a time.
What to Look for When Choosing an EHR Integration Company
Whether you are picking from this list or looking elsewhere, here are simple questions to ask:
- Which EHRs do they actually support today?
Marketing pages claim a lot. Ask for a real list of live, in production connections, not just sandbox or theoretical support.
- Do they support HL7 v2, FHIR R4, X12, and CDA?
Most healthcare data still flows through HL7 v2 messages, and FHIR is the future standard. You almost always need both.
- Is the integration real time or batch?
Care gap alerts, prior authorization, and clinical decision support need real time. Risk adjustment and research can usually live with batch.
- What about TEFCA, Carequality, CommonWell, and the major HIE networks?
As nationwide health information exchange grows, you want a vendor whose network reach matches your needs.
- What are the security and compliance certifications?
HIPAA is the floor. HITRUST and SOC 2 Type II are what you want to see for serious enterprise work.
- How is implementation priced?
Some vendors charge per connection, some per transaction, some per seat, some flat. Get clarity early or budgets blow up later.
- What does support look like once you go live?
Healthcare data outages cost real money and, sometimes, real harm to patients. 24 by 7 monitoring and a clear support escalation path are non negotiable.
Final Thoughts on EHR Integration in 2026
The EHR integration market is busy, and it is only getting busier. Federal rules around interoperability, the rise of AI in clinical workflows, and the steady move toward value based care all mean that healthcare data integration is no longer a nice to have. It is the foundation everything else gets built on.
The simplest way to think about which vendor fits which practice is to match the buyer to the problem:
- Choose Redox if you are a digital health vendor or enterprise platform and your problem is reach. You need to connect to many EHRs without building each pipe yourself.
- Choose Vim if you are a payer or value-based care organization and your problem is clinician adoption. You need data and actions to show up inside the EHR screen, not in a separate dashboard.
- Choose Medbridge if you run a rehab or MSK practice and your problem is delivering education, HEPs, and patient engagement where therapists already work.
- Choose Datavant if you are a health plan, life sciences company, or large health system and your problem is moving and de-identifying records at huge volume for risk adjustment, HEDIS, research, or legal use.
- Choose OmniMD if you are an independent practice or specialty clinic and your problem is vendor sprawl. You want one AI-driven platform that already includes EHR, RCM, telehealth, and patient engagement, with clean external integrations for the things it does not do natively.
If you are evaluating EHR integration companies or EMR integration companies for your own product or organization, the right choice depends on what you are actually trying to do. Start with the use case, not the vendor. Then map the use case to the strengths of these platforms, and you will end up in a much better place than picking the loudest name on a Google search.
The bigger picture is hopeful. Data is finally moving in healthcare. With HL7 integration, FHIR integration, TEFCA, Epic integration paths, and a strong roster of EHR interoperability players, the era of pure data silos is slowly ending. And that is good news for everyone, especially the patients waiting on the other side of all those records.

Wasting Months on Point-to-Point Integrations?
See which integration platform matches your EHR stack, data needs, and team size.

 Written by Dr Girirajtosh Purohit
Written by Dr Girirajtosh Purohit