AI in Medical Billing: Top 5 Platforms Compared (2026)
At a glance
| Platform | Best for | Starting price | Big win | Watch out for |
| CodaMetrix | Big hospitals that want autonomous medical coding | Custom (by volume) | KLAS #1 in autonomous coding for 2026; cuts manual coding work by up to 70% | Costs a lot up front; not for small clinics |
| AKASA | Large health systems that want AI across the whole revenue cycle | Custom (by volume) | AI trained on your own data, with a quote from the chart for every code suggestion | Built for big budgets; not for solo doctors |
| Waystar | Mid-to-large practices that need a broad billing platform | From around $100/month | 98.5%+ first-pass clean claim rate; works with most insurers | Long auto-renewing contracts; mixed support reviews |
| OmniMD | Small to mid practices that want EHR plus billing plus AI in one tool | Custom (by tier) | All-in-one platform; reports a 97% first-pass clean claim rate | Less famous than Waystar or athenahealth at the hospital level |
| athenahealth (athenaCollector) | Outpatient practices that want a managed billing service | Custom; usually 4 to 7% of what you collect | Huge 160,000-provider network feeds the rules engine | Percent pricing gets pricey as you grow; coding work is not fully done for you |
The market for ai medical billing software splits into three buckets. Pick the one that fits your practice and you will save weeks of demo calls.
If you run a hospital or a big health system, you want autonomous coding tools like CodaMetrix or AKASA. They use AI to do the heavy work of medical coding. They sit on top of whatever EHR you already use.
If you run a mid-size or large group, broad billing platforms like Waystar handle claims, payments, and reports for many specialties.
If you run a small or mid-size practice and you are tired of juggling five vendors, all-in-one platforms like OmniMD or athenahealth bundle the EHR, the billing, and the AI in one tool.
How we picked these 5
Here is how we did it. You can use the same checklist when you talk to vendors.
We pulled public product pages, KLAS Research data, Gartner Peer Insights, G2, Capterra, and Software Advice reviews from the last 12 months. Then we scored each one on six things. How real is the AI? How much of the billing process does it cover? What does it connect to? Is the price clear? Who is it built for? And what do real customers say about results?
We also forced ourselves to find at least two honest weak spots for each platform. If a vendor looked perfect, we dug harder. Marketing pages are written to sell. Real users tell you the truth. We trusted the users more.
We did not stick to a strict 1-to-5 ranking, because ‘which is best’ is the wrong question. The right question is ‘which is best for me.’ The order below shows where each tool sits in the market, but the one ranked first is not always the right one for your practice.
OmniMD did not pay anyone to be on this list. No vendor paid us to move up.
Why ai in medical billing actually matters now
Healthy skepticism about ai in medical billing is fair. A lot of vendors rebranded their old rules engines and called it innovation. But the number on the underlying problem has not changed.
The average practice loses 10 to 15 percent of claims to denial – see how that breaks down in our 2026 average claim denial rates by specialty report. Two thirds of those denials never get paid. Each rework costs more than $25 in staff time. And the wait for payment is still 30 to 45 days.
The platforms doing real machine learning, the kind that actually learns from your specific data, are finally moving those numbers. They:
- Read clinical notes the way a smart biller would
- Suggest the right ICD-10 and CPT codes before a claim ever leaves your office.
- Learn how each insurance company behaves over time, and
- Catch problems that humans only spot after a denial.
AI for medical billing is starting to turn billing from a ‘fix it later’ job into a ‘stop it before it happens’ job.
A recent survey found that about 63% of healthcare organizations are already using AI for revenue cycle work. So change is happening. The only real question is which tool fits your practice.
What to look for when you shop for AI medical billing software
There is one test that exposes weak vendor pitches faster than any feature checklist. Pull a denied claim from your last quarter. Hand it to the vendor on the demo call. Ask them, exactly, how their AI would have prevented that specific denial. The platforms doing real work walk you through the reasoning. The ones running rebranded automation change the subject.
If you cannot run that test yet, here are the seven things that actually separate genuine ai medical billing software from the marketing version.
AI that adapts to your specific data.
Some vendors have added ‘AI powered’ labels to older software, and it is worth noticing the difference. The question to keep in mind is whether the system actually learns from your payer mix, your specialty, and your past denial patterns, or whether it applies the same generic rules for every customer. When you ask a vendor what data their AI trains on, a clear and specific answer is a good sign.
Code suggestions you can trace back.
The strongest ai medical coding tools do more than suggest a code. They show you the exact line in the chart that supports it, along with a confidence score. That trail matters more than it might first seem. It helps your team support coding decisions in an audit, and it makes it easier to catch the rare moments when the AI does not get it right.
Prevention, not just detection.
Fixing a denial after the fact is workable, but catching it before submission is where AI really earns its place. It is worth asking vendors how their system flags risky claims before they leave the office. The most helpful tools learn how each insurance company behaves over time and point to the specific issue, rather than a general ‘this might be denied’ alert.
Integration that fits the workflow your team already uses.
When a vendor says ‘we connect to anything,’ that is a good moment to ask for specifics. Which EHRs do they connect to today, in real customer setups, with two-way data flow? It also helps to ask whether the AI sits inside the workflow your team already uses, or whether it asks them to switch between screens throughout the day. The second pattern can quietly slow adoption, even when the underlying tech is strong.
Pricing that fits where your practice is going.
Pricing models vary a lot in this space. Some vendors keep their pricing private. Others charge a percent of what you collect, which means the bill tends to grow alongside your practice. A few charge per provider, which can feel more predictable. It helps to run the math for where your practice will likely be in two years, not just where it is today. A pricing model that does not match your growth plans can add up to a meaningful cost over the life of a contract.
Compliance you can audit, not just trust.
HIPAA, SOC 2, and HITRUST are the baseline you would hope for from any healthcare vendor. Beyond those certifications, it is worth asking whether the vendor keeps an audit trail for every AI decision, watches for changes in payer rules and CMS guidance, and can support you if a payer audit comes up. It is also fair to ask how patient data flows through their AI, since general-purpose models like ChatGPT were not designed with healthcare in mind.
A free audit before you sign anything.
One of the most helpful things a vendor can offer before a contract is a free billing audit on your actual claim data. An audit shows you, in real numbers, what their AI would have caught for you. It also gives the vendor a chance to demonstrate value in your real environment, instead of just in a polished demo. If a vendor is not willing to run one, it is worth understanding why.
1. CodaMetrix: the coding specialist
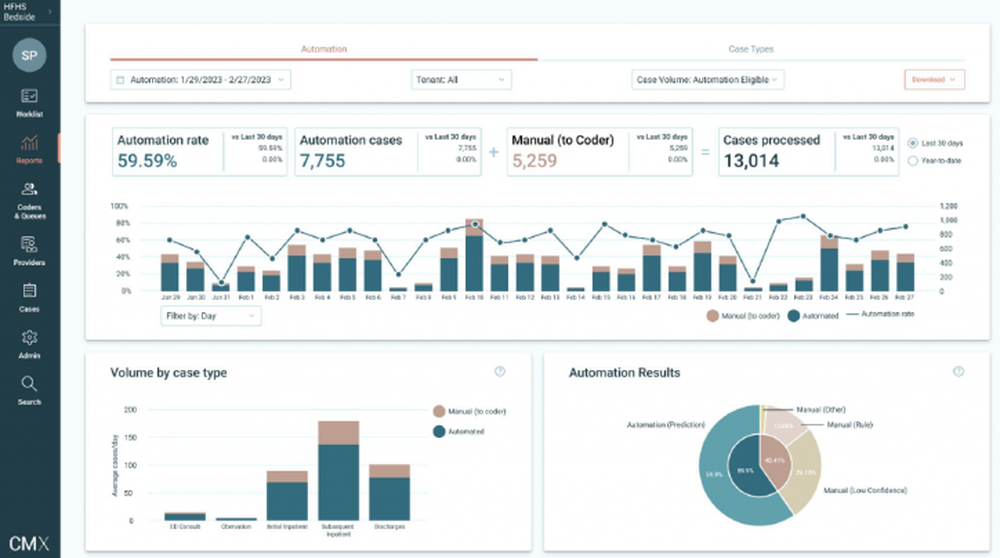
CodaMetrix is one of the most respected ai medical coding companies right now. KLAS Research named it the #1 solution in the brand-new 2026 Best in KLAS award for autonomous medical coding. Its customer list reads like a top-10 of US hospitals: Mass General Brigham, Mayo Clinic, Yale Medicine, Henry Ford Health, the University of Colorado.
If your hospital runs Epic and your coding team is buried, this is the first vendor on your list.
What it does
CodaMetrix is small on purpose. It does not sell a full billing platform. It does one thing well. It is a pure medical coding AI tool. It reads clinical notes, imaging reports, and procedure data, and it picks the right ICD-10, CPT, and HCC codes with very little human help. Coders go from typing codes all day to checking the AI’s work. That is a much better job, and it helps with the national coder shortage.
What it does well
The outcomes are real, and they come from named customer case studies.
- CodaMetrix reports cutting coding costs by 60 percent.
- Cutting manual coding work by 70 percent.
- Dropping claim denials by up to 60 percent.
- And speeding up time to cash by 5 weeks.
Hospitals using its radiology product report turning around codes in about 4.8 days. Before, it took over 43 days. The 2026 KLAS #1 rating adds outside proof you cannot fake.
The Epic Toolbox approval is also a big deal. It means CodaMetrix meets Epic’s official integration guidelines. So if you run Epic, set-up is much faster.
Where it falls short
I will not pretend this is for everyone. Real customer reviews on Gartner Peer Insights flag three things:
- Hooking it up to older EHRs can be a pain.
- The price is heavy for smaller groups.
- And it does not customize well for niche workflows.
A 5-doctor primary care clinic should not buy this. Full stop.
Pricing
Custom, based on how many cases you process and how big your group is. They do not post numbers. You have to ask for a quote.
Best for
Big hospitals, academic medical centers, and large multi-specialty groups running Epic, Oracle Health (Cerner), or other big-system EHRs.
2. AKASA: AI across the whole revenue cycle
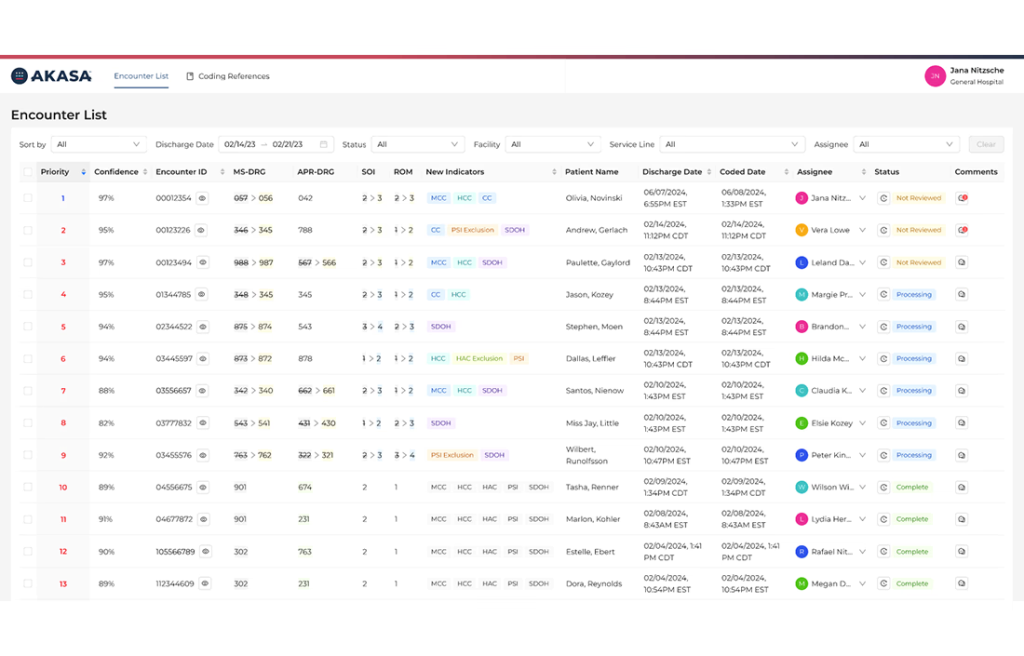
If CodaMetrix is the coding expert, AKASA is the wider tool. It serves more than 650 hospitals and 6,500 outpatient sites in all 50 states. It covers prior authorization, claim status, clinical documentation help, and coding. It is one of the biggest names in artificial intelligence medical billing at the hospital level.
What it does
AKASA trains an AI model on your own clinical and money data. Then it puts that AI right into your team’s daily workflow. The AI reads charts. It logs into insurance company portals. It fills out prior authorizations. It checks on claim status. And it spots coding chances your team missed. Your staff stays in their normal EHR the whole time.
A few of the specific tools worth knowing:
- Coding Optimizer looks at codes you already submitted and finds revenue and quality measures you missed
- Authorization Advisor helps with prior authorizations, the task most billers would happily set on fire
- Claim Status Manager checks on claims at the insurance company and updates the EHR for you, so your staff does not have to log into 50 different portals every day
Every code suggestion comes with a quote from the chart that backs it up. Most other tools are more of a black box. AKASA shows its work.
What it does well
AKASA’s models reportedly beat general AI models like GPT-4 by up to 40 percent on health-system tasks. That is because they train on your data, not on the open internet.
Real customers report a 13 percent drop in A/R days and over 300 staff hours saved per month. The HIPAA, HITRUST, and SOC 2 certifications are all in place.
If you want generative AI but you also need to see how it makes its choices, AKASA is one of the few that opens the box.
Where it falls short
Two things to call out.
First, it is built for big systems. Pricing is tied to how much you process. That works for hospitals. It does not work for solo doctors or small clinics.
Second, the AI is only as good as your data. If your clinical notes are messy, the AI inherits the mess. Garbage in, slightly smarter garbage out.
Set-up usually takes around four months. So this is a strategic move, not a quick fix.
Pricing
Custom, not posted. Plan for a real monthly bill if you are a mid-to-large health system.
Best for
Mid to large health systems that already have a strong EHR, a real revenue cycle leader on staff, and the budget for a four-month rollout.
3. Waystar: the steady mid-market choice
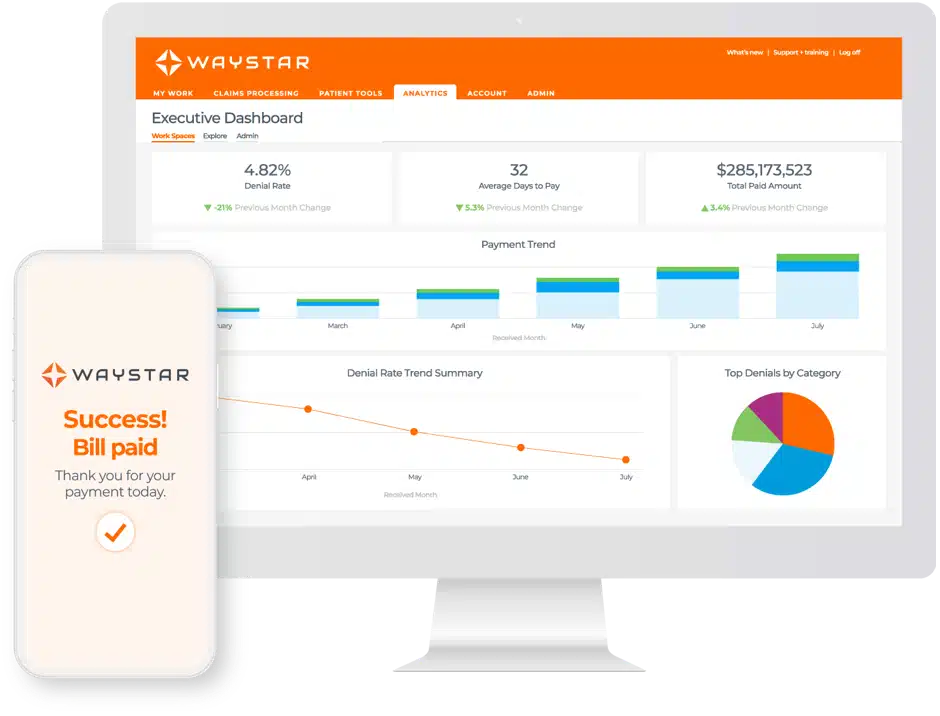
Waystar (Nasdaq: WAY) started in 2017 when Navicure and ZirMed merged. Today it processes over 6 billion healthcare payment transactions a year and serves more than a million providers. It has been doing ai revenue cycle management work since before ‘AI’ became the hot word.
What it does
Waystar is full-service. It handles eligibility checks, charge capture, claim submission, payment posting, denial work, and reports, all in one cloud platform. Its newer AI features sit under the AltitudeAI brand. They focus on guessing which claims will be denied and finding money insurers took back.
In April 2026, Waystar launched what it calls the first AI tool for ‘silent denials.’ That is a category where insurers reportedly take back more than $40 billion a year in payments providers never knew were missing.
The Claim Manager product reports a 98.5 percent first-pass clean claim rate. That is one of the highest in the industry. Eligibility checks, claim status, payment posting, patient payment plans, and custom reports are all in the box.
What it does well
Waystar’s biggest advantage is its size. Hospitals, doctor groups, surgery centers, labs, and nursing facilities all use it. The clean claim rate is real and well documented. AnMed Health reports collecting an extra $931K using Waystar. Renown Health says it cut A/R days in half.
If you want a vendor who has seen your specific insurance company in your specific state a thousand times, this is a safe pick.
Where it falls short
Read the recent G2 and Capterra reviews and three complaints come up over and over.
Customer support is hit or miss. Several users describe cases that got closed before anything was actually fixed. One Software Advice reviewer put it bluntly: the reps just want to close the case, not actually fix the problem.
Pricing is not clear up front. Waystar does not publish numbers, and a widely-shared Capterra review describes a 24-month auto-renewal with a 200 percent price hike at renewal time, despite a contract cap of 5 percent.
The contract terms are the part to watch. Pricing is reported to start around $100 per month. But the full suite costs much more. And the renewal language has burned more than one practice. Read every line before you sign.
Pricing
Subscription-based. Tailored by group size and which modules you pick. Reported entry price near $100 per month. Full enterprise contracts run much higher.
Best for
Mid to large practices, hospital systems, and billing companies that want one platform for claims, payments, and reports. You should also have someone in-house who can manage the set-up and the contract.
4. OmniMD: the all-in-one for small and mid practices
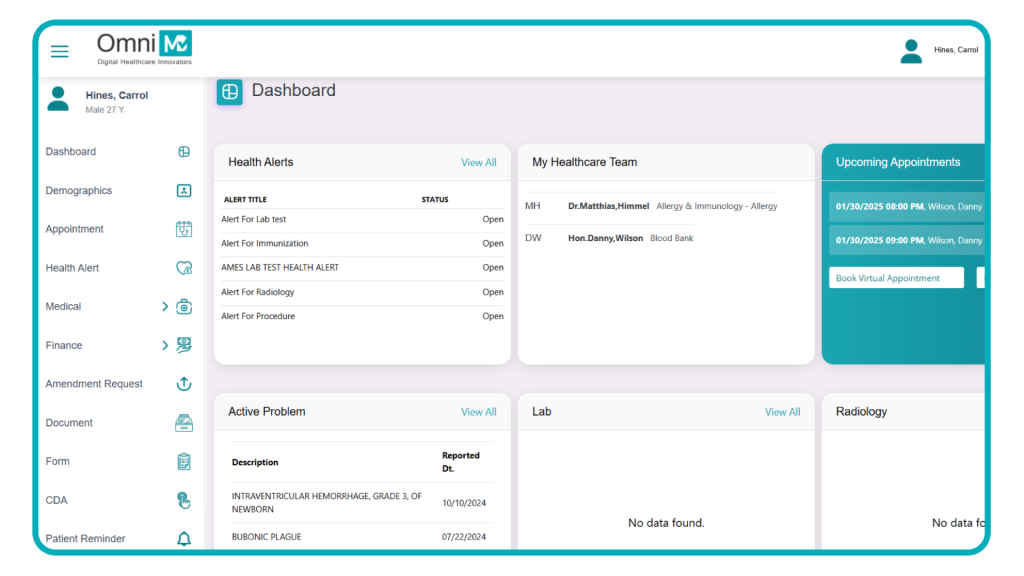
OmniMD is the platform we build. So the easy move would be to talk it up. We are not going to do that. We will give you the same balanced view we gave the others, including the not-so-great parts.
What it does
OmniMD is an all-in-one US platform. Our EHR, AI medical billing tool, medical billing service, and patient tools all live inside the same product. That matters most for practices that do not want to manage four vendor relationships.
One thing we want to be upfront about. Even though we are an all-in-one platform, our approach is highly customized. We do not push every practice into the same template. We tune the workflows, coding rules, dashboards, and reporting to how your practice actually runs.
And if the full suite is not what you need, that is fine too. Plenty of our clients use these services independently. Some bring us in only for medical billing. Some plug our ai medical billing tool into the EHR they already use. Some keep billing in-house and use our coders for specific specialties only.
We have built a strong reputation in those standalone engagements, not just in the all-in-one rollouts. So whether you want one piece, two pieces, or the whole thing, the customization is the same.
Our ai medical billing tool uses machine learning to spot likely denials before submission. It also handles eligibility checks and prior authorizations, and it learns how each insurance company acts over time. Coding, claims, and payments all live in one workflow.
For practices that would rather hand the whole thing off, we also offer a managed medical billing service. That comes with certified coders and a dedicated account manager.
A few features worth flagging:
- AI denial prediction based on each insurance company’s history
- Real-time dashboards for AR days, denial rate, net collection rate, clean claim rate, and DNFB
- Specialty-tuned coding for cardiology, pain management, behavioral health, and others
- Connects to most major third-party EHR and practice management systems, alongside the native OmniMD EHR
- HIPAA-compliant, with an API-first setup
What it does well
We report a 97 percent first-pass clean claim rate across our billing services. New clients in some specialties see a 20 percent revenue increase in the first 90 days. Real customers, like Dawn K. Walker (a family practice owner) and the team at Solid Sobriety, describe big drops in claim denials and better collections.
The biggest practical win is the all-in-one setup when clients choose it that way. One login. One vendor. One support team for the EHR, the billing, and the patient tools. If you have ever been on a three-way call with your EHR vendor, your billing vendor, and your clearinghouse trying to figure out why a claim got rejected, you know why this matters.
That said, the customization piece is what most clients tell us made the difference. The platform is one thing. The way it gets shaped to your practice, your specialty, and the specific tools you actually need is what moves the numbers.
Where it falls short
We do not have the brand name of Waystar or athenahealth at the hospital level. Outside reviews on G2 and Capterra are thinner than for the big brands, so it is harder for buyers who want to verify everything from outside sources.
Pricing
Custom, based on practice size, specialty, and the modules you actually want, whether that is the full platform or just one or two services. We also offer a free billing audit, which is a useful no-risk first step no matter which vendor you end up picking.
Best for
Independent practices, small to mid multi-specialty groups, and growing clinics that want one platform with AI built in. Also a strong fit for practices that want just one or two of these services on a standalone basis, with the option to expand later. Less of a fit for buyers who want a stack of completely separate generic tools and zero customization.
5. athenahealth athenaCollector: the network-driven choice
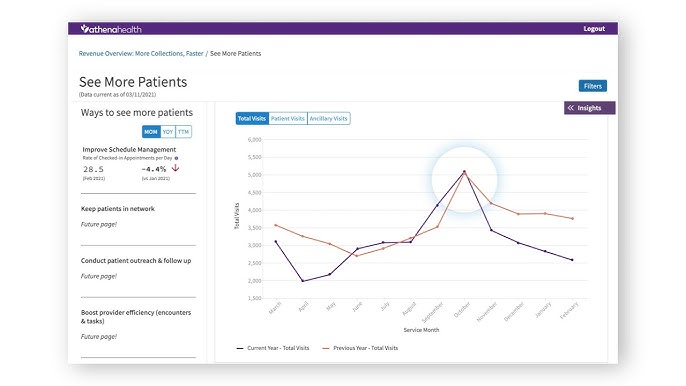
athenahealth has been a cloud-based vendor since 1997. So it is one of the only big outpatient EHRs that did not have to bolt the cloud onto an old desktop product. Its athenaCollector tool is the billing piece of the bigger athenaOne platform. The company is leaning hard into newer artificial intelligence medical billing features. It says it wants to cut doctors’ billing work by 50 percent.
What it does
athenaCollector handles the full billing process. Scheduling, eligibility, claim submission, denial work, and payment posting. Its big differentiator is the athenaOne Network. That network connects more than 160,000 providers and 72 million patients.
Data from that network feeds a rules engine with over 29,000 billing rules. Athena makes more than 4,500 rule changes a year.
So when an insurance company changes a rule, every practice on the network benefits. That is a real network effect. Most competitors cannot match it.
What it does well
The network is the moat. Every new provider who joins makes the rules engine smarter for everyone else.
- athenaCollector ranks at the top of independent reviews year after year.
- athenahealth was named Best in KLAS for independent outpatient practices in 2025.
- First-pass acceptance rates above 95 percent are common.
Athena even backs them with a money-back guarantee tied to the number.
The pricing model also gets credit for being fair. It is performance-based. So athenahealth only earns more when you collect more. The incentives line up.
And athena is one of the very few vendors that lets practices cancel any time. That is rare in this industry.
Where it falls short
Three issues come up in real reviews.
First, percent-based pricing (usually 4 to 7 percent of what you collect) gets very expensive as your practice grows. One verified reviewer called it “the Cadillac of EMRs” but said the price became a problem at higher volumes.
Second, the coding service is not fully complete. You will still need an in-house biller or coder. That detail surprises a lot of buyers.
Third, customer support has mixed reviews. Some users report slow responses and cases that take days to escalate. The interface also feels cluttered to some users.
Pricing
Two main models.
- Percent-based, usually 4 to 7 percent of what you collect. Or per encounter.
- Some users report a starting price near $140 per provider per month. Real cost depends on volume and which modules you pick.
Best for
Independent outpatient practices, especially newer ones, that want a hands-off billing service and the safety of a big national network.
Less ideal for high-volume groups trying to control costs.
How to actually pick one
Most demo discussions usually come down to four key questions. Work through them step by step, and your shortlist will narrow quickly.
Question 1: How big is your practice and what EHR do you use?
Run a hospital or large health system on Epic or Oracle Health (Cerner)? Look at CodaMetrix or AKASA for autonomous coding. They sit on top of your existing billing platform.
Run an independent practice or a small to mid group? OmniMD or athenahealth give you one tool that does it all.
Run a mid-market group that needs a strong clearinghouse? Waystar is a safe pick.
Question 2: Do you need coding, full billing, or both?
Coding-only tools like CodaMetrix and AKASA leave the rest of the billing process to your other tools. Full billing platforms like Waystar, athenaCollector, and OmniMD cover claims, payments, and patient billing too.
Buying coding-only when you need full billing leaves you taping tools together.
Buying full billing when you only need coding wastes money.
Pick a side before you take a single demo.
Question 3: How predictable does the bill need to be?
Practices on tight margins should be careful with percent-of-collections pricing. As your collections grow, your monthly bill grows too. Sometimes faster than you can hire to handle the work.
Per-provider or per-volume pricing is more predictable. Even if the up-front number looks bigger.
Question 4: How much set-up time can you handle?
CodaMetrix and AKASA usually take four months or more to set up. Waystar has a steep learning curve. OmniMD and athenahealth offer guided onboarding for smaller, mid-sized, and large practices.
If you do not have someone on staff to lead this, pick a platform with hands-on onboarding. Even if it shrinks your shortlist.
A practical move: Start with a free billing audit. (OmniMD, Waystar, and others offer one.) Use what the audit finds to test two of your top picks in a 30 to 60 day pilot. Then commit.
Do not sign a multi-year contract before you have run real claims through the system. Vendors who refuse to pilot on your own data are the ones to worry about.
The Final Word
The market for ai medical billing is not new or risky anymore. Every platform on this list runs in real practices today, serving thousands of providers. The differences are about fit. Not about whether the tech works.
Run a big health system on Epic? CodaMetrix and AKASA will move the needle on coding cost and denial rates faster than anything else.
Mid-size group looking for a broad billing platform? Waystar is the safe, proven default.
Small or mid practice that wants to cut down on vendors and put AI to work without a six-month set-up? OmniMD and athenahealth are the most realistic picks. OmniMD tends to fit specialty groups and growing clinics. athenahealth tends to fit outpatient practices that want a managed service.
Whichever way you go, run a billing audit with two or three vendors first. Ask for live demos using your own claim data. Read the contract, especially the renewal section. Then sign.
If you want to start with OmniMD’s free billing audit, you can request one here.
FAQs
Will AI replace medical billers and coders?
Not anytime soon. Every real vendor in this space, including CodaMetrix and AKASA, calls their AI a co-pilot. Not a replacement.
The AI handles the boring, repeat tasks. Reading notes. Suggesting codes. Checking eligibility. Your humans handle the weird cases, the appeals, and the quality checks.
The bigger shift is productivity. One good biller can now do the work of three. The job changes. It does not vanish.
How accurate is ai medical coding today?
Top tools report autonomous coding accuracy above 95 percent for routine cases. Some report over 99 percent for narrow specialties like radiology.
Accuracy drops on complex inpatient cases. So most ai in medical coding tools send low-confidence cases to a human coder.
When you talk to a vendor, ask for accuracy by specialty. Not just one big average. A tool that codes radiology at 99 percent and behavioral health at 78 percent is really two products in one.
Is AI medical billing software HIPAA compliant?
It needs to be. The leading platforms publicly confirm HIPAA compliance, SOC 2 certification, and HITRUST certification. If a vendor is missing one, ask why.
Also ask how they train the AI. General AI models like ChatGPT typically should not see your patient data. Training should either be done on data with patient names stripped out, or on your data inside a secure space just for your group. Get the answer in writing.
How long does set-up take?
It depends.
Big tools like CodaMetrix and AKASA usually take four months or more. That includes a quiet phase where the AI watches your team’s workflow before it starts making suggestions.
Waystar can take several weeks to fully set up.
All-in-one platforms like OmniMD and athenahealth often go live for small practices in 4 to 11 weeks.
Two to three months is a fair planning window.
What is the real ROI of ai for medical billing?
Numbers vary. But the patterns are pretty consistent.
Coding cost drops of 30 to 50 percent. Denial drops of 30 to 60 percent. A 5-to-1 ROI over five years is what most ai medical coding companies report.
Practices using full ai medical billing software often report 20 percent revenue jumps in the first 90 days. Mostly from catching missed charges and stopping early-stage denials.
The only real way to check this for your own practice is a free billing audit on your own claims. Vendor case studies are nice. Your own numbers are what matter.
Can a small practice actually afford this?
Yes, if you pick carefully.
Big tools like CodaMetrix and AKASA are not built for small practices. Trying to make them work will burn money and time.
All-in-one platforms like OmniMD and athenahealth offer entry-level tiers that small clinics can afford. Waystar’s reported entry price of around $100 per month is real, though the full suite costs more.
The biggest risk for small practices is signing a long contract before testing the tool. Always pilot first.
Do I need to replace my EHR to use this?
Usually no.
Coding-first tools like CodaMetrix and AKASA are built to work with major EHRs, especially Epic and Oracle Health (Cerner). No rip-and-replace needed.
Waystar connects to most EHRs through standard interfaces.
OmniMD works the same way for practices that want it to. Its billing, coding, RCM, and prior auth services run as standalone modules that plug into your existing EHR, or you can use it as a full all-in-one platform if that’s the better fit.
The exception is platforms like athenahealth, where the EHR and the billing tool are the same product. In that case, a switch is part of the deal. But it is planned for, supported, and not the painful all-or-nothing event it used to be.

Your Billing Team Deserves a Smarter Workflow
5 AI platforms compared – find the one that plugs directly into your revenue

 Written by Dr Girirajtosh Purohit
Written by Dr Girirajtosh Purohit